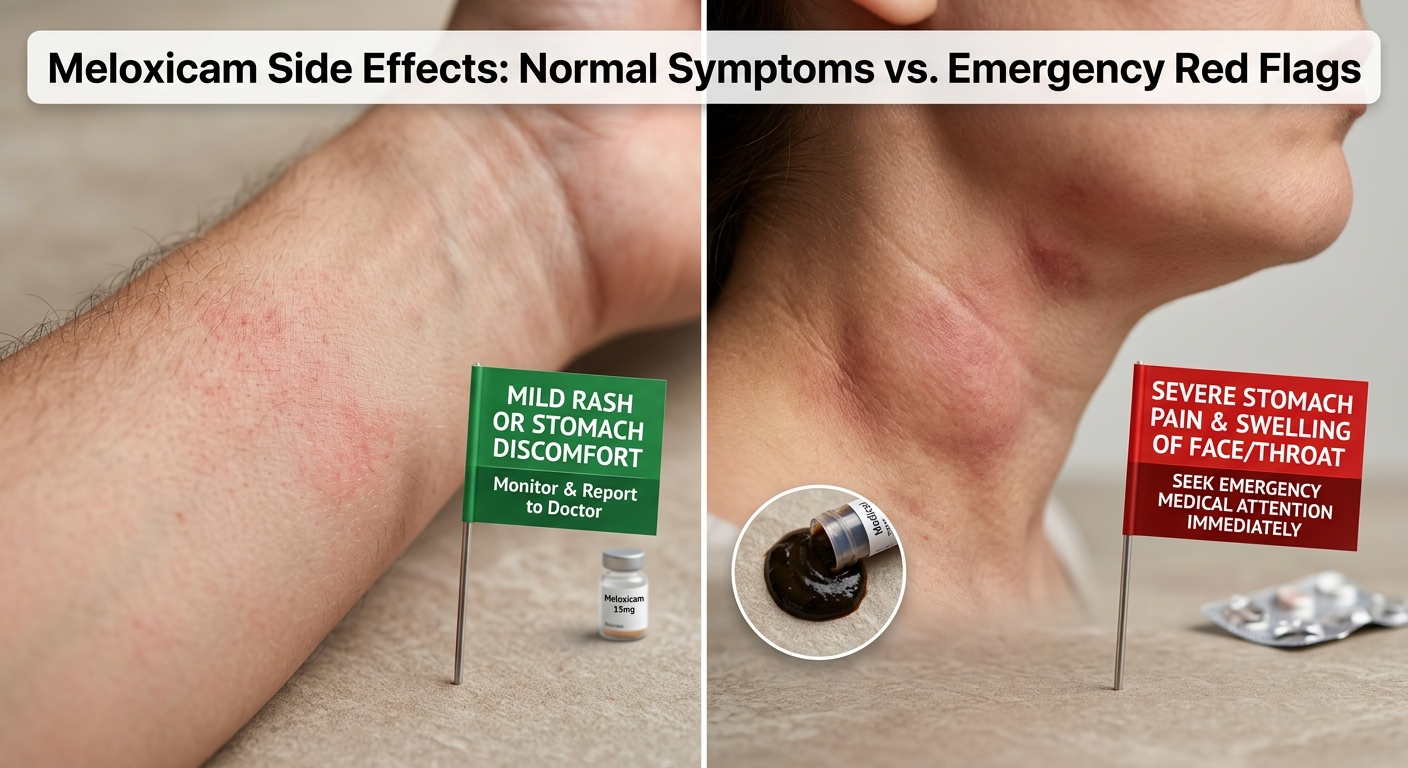
Meloxicam Side Effects: Normal Symptoms vs. Emergency Red Flags
By Frankie Sze | 5/2/2026
Introduction: Understanding Your Body’s Response to Meloxicam
When initiating treatment with meloxicam, it is essential to recognize that you are beginning a course of a potent, long-acting nonsteroidal anti-inflammatory drug (NSAID). As noted by experts, “Meloxicam is a long-acting medicine that only needs to be given once a day,” typically in dosages ranging from 7.5 mg to 15 mg to manage chronic arthritis pain (Drugs.com). Because the medication remains active in your system for an extended period, your body requires a brief period of adjustment. Understanding what to expect can help you navigate this transition, and you can learn more about managing your regimen in our guide, Meloxicam 101: Your Daily Guide to Steady Joint Relief.
It is perfectly normal to experience mild initial sensations as your system adapts. You may notice temporary dizziness, which often subsides within minutes or hours, or headaches that may persist for 12 to 24 hours. Some patients also report painless ankle swelling, a byproduct of fluid retention common with NSAID use, or minor stomach upset. While these common reactions are typically manageable, they are part of a broader safety profile established during clinical trials. This profile highlights the importance of current medical guidance: patients should utilize the lowest effective dose for the shortest duration possible to mitigate long-term risks, such as cardiovascular events, heart attack, stroke, or the development of silent gastrointestinal ulcers and bleeding. Furthermore, due to risks such as reduced amniotic fluid, NSAIDs should generally be avoided after the first trimester of pregnancy.
As we monitor these factors through ongoing pharmacovigilance, remember that while mild adjustments are standard, you must remain vigilant. Serious allergic reactions like anaphylaxis, which can lead to rapid airway closure, require immediate emergency intervention. By staying informed and communicating closely with your physician, you can better manage your body’s response while seeking consistent relief.
The Green Zone: Common Mild Side Effects and What to Expect
When initiating meloxicam, a long-acting NSAID typically prescribed at daily doses of 7.5 mg to 15 mg, it is common for the body to experience a transitional period. As clinical literature notes, “Common side effects include stomach upset, headaches, and dizziness.” According to clinical insights into meloxicam safety profiles, these mild reactions are generally manageable and often transient.
Understanding the expected timeline for these symptoms can help patients navigate the early stages of treatment. Dizziness is frequently reported as a fleeting sensation that typically resolves within minutes to hours. Headaches, while slightly more persistent, generally subside within a 12-24 hour window. Additionally, some patients may notice painless ankle swelling, known as edema, which occurs due to the mild fluid retention associated with NSAID use.
While these mild side effects are well-documented from clinical trials established prior to FDA approval, they should be monitored closely. Current medical guidance emphasizes using the lowest effective dose for the shortest duration possible to mitigate risk. If you encounter symptoms that persist beyond these expected timeframes or if you experience significant discomfort, consult your healthcare provider to discuss whether an adjustment to your treatment plan is necessary.

The Yellow Zone: When to Monitor and Mention Symptoms to a Pharmacist
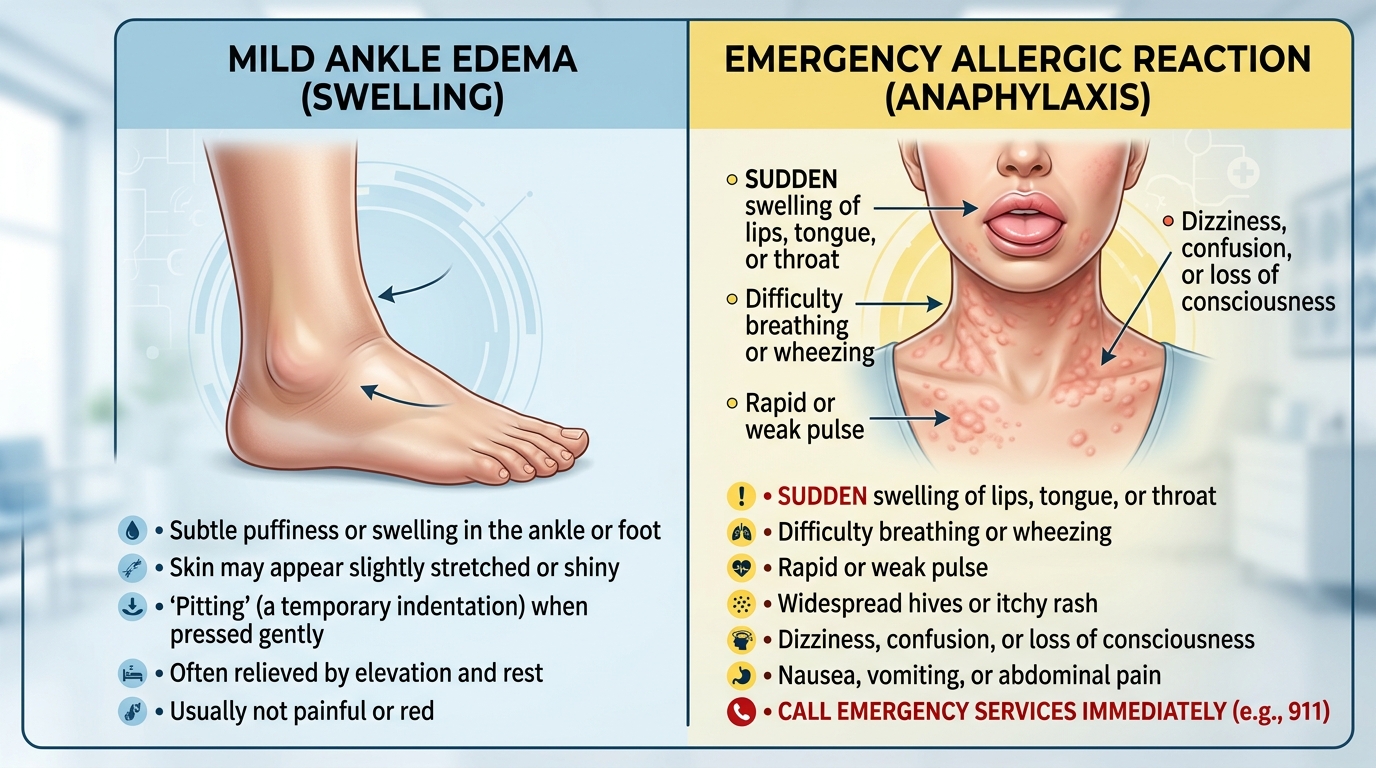
Navigating the side effects of a long-acting NSAID like meloxicam requires a keen ability to distinguish between benign, cumulative physical changes and acute, life-threatening events. While meloxicam is generally effective for arthritis pain when dosed once daily at 7.5 mg to 15 mg, its mechanism of action can lead to systemic shifts. A common, typically painless development is pedal edema—swelling in the legs and ankles—which occurs due to fluid retention. As noted in clinical guidance, “Some people may notice swelling in their legs and ankles while taking meloxicam. This isn’t unusual with NSAIDs, since they can cause you to retain fluid” (GoodRx). While this fluid retention is a common side effect, it warrants a conversation with your pharmacist or physician during your next check-in, particularly to ensure it does not coincide with cardiovascular symptoms.
In contrast, the “Red Zone”—an immediate emergency—is characterized by sudden, severe manifestations. Unlike the gradual onset of fluid retention, serious allergic reactions such as anaphylaxis can trigger airway closure within minutes. Patients must understand this temporal difference: mild side effects like dizziness often subside within minutes to hours, and headaches typically resolve within 12 to 24 hours, but difficulty breathing, hives, or rapid facial swelling require immediate emergency intervention. Furthermore, while the current standard of care emphasizes using the lowest effective dose for the shortest duration to minimize cardiovascular risk and potential GI issues like silent ulcers or bleeds, ongoing pharmacovigilance reminds us that patient awareness remains the most critical layer of safety. Always prioritize reporting persistent or sudden changes to your clinical team, as these distinctions are vital for long-term safety monitoring.
The Red Zone: Emergency Warning Signs Requiring Immediate Medical Care
While clinicians advise utilizing the lowest effective dose of meloxicam for the shortest duration to manage arthritis pain, patients must remain vigilant regarding “The Red Zone”—a set of acute symptoms that signal severe systemic distress. Although common mild side effects like stomach upset, headache, or dizziness—which typically subsides within hours—are manageable, the drug’s pharmacological profile requires immediate attention to signs of major cardiovascular or gastrointestinal events. Because meloxicam carries intrinsic risks of gastrointestinal bleeding and ulcers that can manifest without warning, users must monitor their digestive health closely.
The Oceans Luxury Rehab clinical summary explicitly states: “Seek emergency care if you experience chest pain or pressure, sudden weakness on one side of your body, trouble speaking or understanding speech, vomiting blood or material resembling coffee grounds, black or bloody stools, severe shortness of breath or trouble breathing, swelling of your face or tongue.” These symptoms may indicate an impending heart attack, stroke, or severe allergic reaction (anaphylaxis), which can lead to airway closure within mere minutes.
Furthermore, while painless ankle swelling is a known, common side effect of fluid retention, it must be differentiated from systemic respiratory distress. As clinical research and ongoing pharmacovigilance continue to refine the understanding of long-term cardiovascular risks, patients should recognize that any neurological or cardiac anomaly necessitates urgent medical intervention. By adhering to these emergency protocols, patients can mitigate the risks identified in long-term safety profiles, ensuring that life-saving measures are taken before minor complications escalate.
Patient Empowerment: How to Document and Report Your Symptoms effectively
Effective communication is the cornerstone of safe pain management. As you navigate your treatment plan, as outlined in Meloxicam 101: Your Daily Guide to Steady Joint Relief, maintaining a detailed symptom log is essential. Meloxicam, a prescription-only, long-acting NSAID typically dosed once daily at 7.5 mg to 15 mg, requires diligent self-monitoring. While clinical trials established the baseline safety profile regarding common gastrointestinal and cardiovascular risks, your personal observations provide the data necessary for ongoing pharmacovigilance.
When documenting, be precise about duration and severity. Common mild effects like stomach upset, headache, and dizziness are frequent; however, temporal patterns matter—dizziness often subsides within minutes to hours, while headaches may persist for 12-24 hours. Furthermore, keep track of physical indicators such as painless ankle swelling, or edema, which is a hallmark of NSAID-induced fluid retention. It is imperative to be vigilant for silent risks, such as gastrointestinal bleeding or ulcers, which can emerge without warning. Due to long-term cardiovascular risks—including stroke and heart attack—or specific contraindications like pregnancy after the first trimester, you must immediately report any severe symptoms, particularly signs of anaphylaxis like airway closure, which requires emergency intervention.
You are an active partner in your care. Physicians currently emphasize using the lowest effective dose for the shortest duration to balance relief and safety. When you experience side effects, utilize the official reporting guidelines provided by US Pharmacist: “Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.” By documenting your experiences, you contribute to the future refinement of safety warnings for all patients, ensuring that therapeutic outcomes remain both effective and secure. — Frankie Sze.