Mixing Meloxicam with Other Pain Relievers: The Stacking Danger
By Frankie Sze | 5/2/2026
The One-NSAID Rule: Why Stacking is a Safety Hazard
When managing chronic inflammation, the distinction between prescription-strength medications and over-the-counter options can sometimes blur, leading to dangerous clinical assumptions. Meloxicam was originally developed as a more COX-2 selective NSAID, designed specifically to reduce the high incidence of gastrointestinal distress associated with older agents like aspirin and ibuprofen. However, despite its specialized design, it remains firmly within the non-steroidal anti-inflammatory drug family. As we explore in Meloxicam 101: Your Daily Guide to Steady Joint Relief, maintaining a consistent therapeutic level is essential for joint relief, but attempting to supplement this regimen with additional NSAIDs is a critical safety error.
Patients often mistakenly view these medications as complementary supplements rather than competing agents. In reality, combining a long-acting NSAID like meloxicam—typically dosed once daily at 7.5 mg to 15 mg—with a short-acting agent like ibuprofen, which has a half-life of only two hours, results in an unsafe drug overlap. According to experts at Ikon Recovery Centers, “No. These drugs are both NSAIDs and perform similar functions. Therefore, they should not be combined.” Attempting to treat breakthrough pain by stacking these medications significantly elevates the risk of life-threatening gastrointestinal bleeding, stomach ulcers, and acute kidney damage.
This risk is further compounded by the modern prevalence of multi-symptom “PM” or “Cold” products, such as Advil PM, Aleve Cold, and Motrin Cold, which often contain “hidden” NSAIDs that patients ingest without realization. To ensure clinical safety, a 24-hour washout period is strictly recommended when transitioning between ibuprofen and meloxicam. For those needing management for breakthrough pain, acetaminophen remains a safer alternative, provided the daily intake stays well below the 3,000 mg to 4,000 mg threshold. While the future of pain management may shift toward topical NSAIDs to mitigate these systemic risks, current practice mandates the strict adherence to the one-NSAID rule.
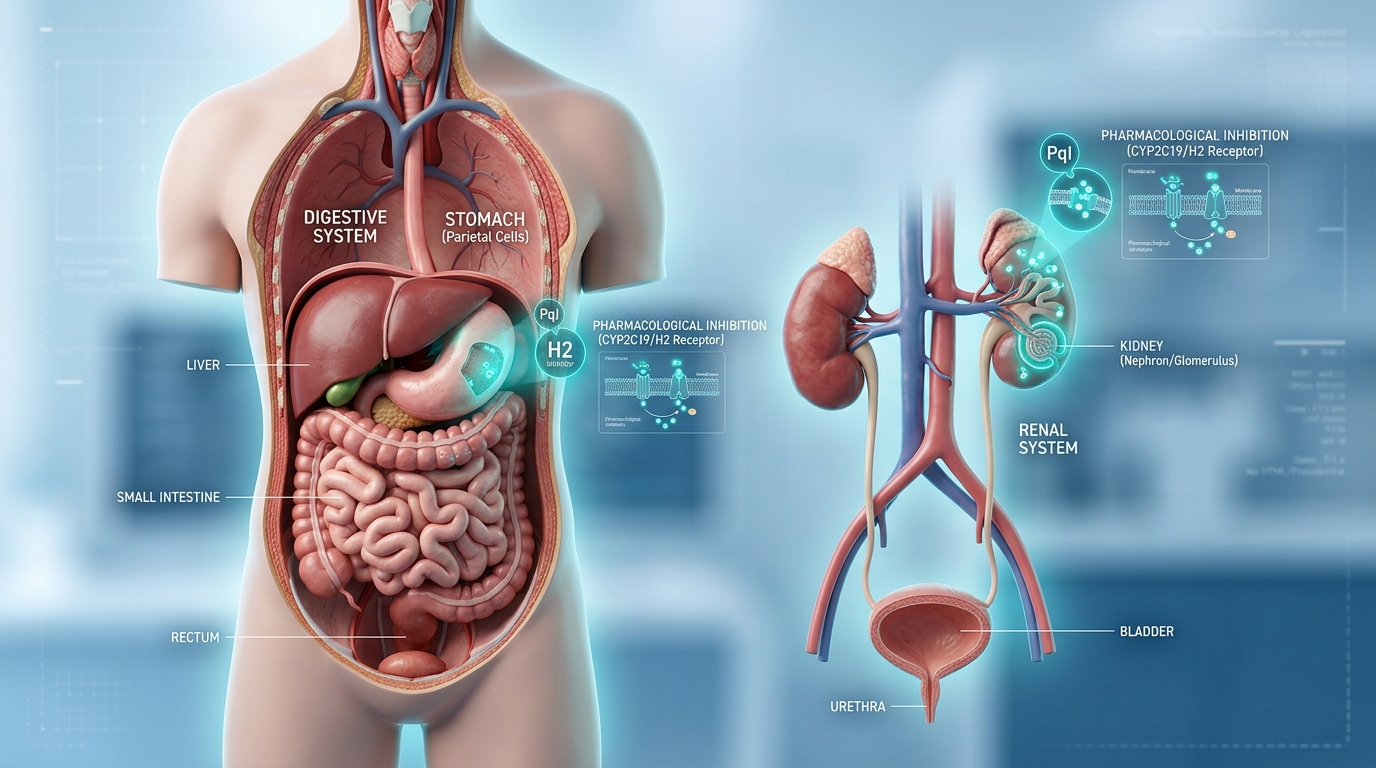
Mechanism of Injury: How Doubling Up Damages the Stomach and Kidneys
To understand why combining nonsteroidal anti-inflammatory drugs (NSAIDs) is hazardous, one must look at the physiological role of prostaglandins. These lipid compounds serve as vital chemical messengers that maintain the integrity of the gastric mucosa and regulate renal blood flow. Meloxicam was originally developed as a COX-2 selective agent specifically to minimize the gastric irritation common with older, non-selective NSAIDs like ibuprofen. However, when patients inadvertently stack medications—often by combining a daily 7.5 mg or 15 mg meloxicam dose with multi-symptom products like Advil PM, Aleve Cold, or Motrin Cold—the systemic inhibition of protective prostaglandins reaches a critical threshold.
Because ibuprofen has a short half-life of approximately two hours, requiring frequent dosing, it is often the catalyst for accidental overlap. A 24-hour washout period is clinically recommended when transitioning therapies to prevent this cumulative toxicity. As noted by experts, “Because both medications are NSAIDs, taking them together increases the risk of side effects, such as stomach ulcers, gastrointestinal bleeding, or kidney damage.” By stripping the stomach of its bicarbonate-rich protective barrier and simultaneously inducing renal vasoconstriction, the body loses its primary defense mechanisms. While safer alternatives for breakthrough pain exist—such as acetaminophen, provided daily intake remains strictly below the 3,000 mg to 4,000 mg limit—the systemic risks associated with NSAID stacking remain a pressing concern for patient safety.
Hidden Risks: Identifying NSAIDs in Multi-Symptom OTC Products
While modern pharmacology initially pursued drugs like meloxicam as more selective COX-2 inhibitors to mitigate the gastrointestinal distress frequently caused by traditional NSAIDs like ibuprofen, the current clinical landscape faces a different challenge. Patients are increasingly relying on multi-symptom products—specifically ‘PM’ sleep aids and cold-relief formulations—that often contain ‘hidden’ NSAIDs, leading to a dangerous trend of accidental drug stacking. Products such as Advil PM, Aleve Cold, and Motrin Cold can quietly contribute to a patient’s total daily dose, unknowingly pushing them beyond safe therapeutic limits.
This is particularly hazardous given the distinct pharmacokinetic profiles of these medications. Ibuprofen has a short half-life of approximately two hours, typically requiring dosing every four to six hours, whereas meloxicam is a long-acting NSAID usually dosed once daily at 7.5 mg to 15 mg. If a patient transitions between these medications without caution, the risk of overlap increases significantly. Consequently, a 24-hour washout period is recommended when switching from ibuprofen to meloxicam to prevent potential toxicity. Stacking these agents substantially heightens the risk of severe adverse events, including gastrointestinal bleeding, stomach ulcers, and acute kidney damage.
As GoodRx notes, “Keep in mind that NSAIDs are often included in OTC cold and flu medications and sleep aids. Check the label carefully or ask a pharmacist for assistance.” For those managing chronic pain, clinicians often suggest that acetaminophen remains a safer option for breakthrough pain alongside meloxicam, provided the total daily intake is kept strictly under 3,000 mg to 4,000 mg. Looking toward the future, ongoing research into topical NSAIDs may eventually provide a more localized, systemic-sparing method of pain management, reducing the reliance on these problematic oral multi-symptom cocktails.

Managing Breakthrough Pain: Safe Alternatives to NSAID Stacking
For patients managing chronic conditions with meloxicam—a long-acting NSAID typically dosed once daily at 7.5 mg to 15 mg—the temptation to supplement with over-the-counter options during breakthrough pain is common but fraught with danger. Because ibuprofen carries a short half-life of approximately two hours and requires frequent dosing every four to six hours, patients often inadvertently engage in NSAID stacking. This practice drastically increases the risk of gastrointestinal bleeding, gastric ulcers, and acute kidney injury. It is critical to note that if a provider recommends switching from a short-acting agent to meloxicam, a 24-hour washout period is essential to prevent dangerous drug overlap.
The modern landscape of self-medication complicates this further; many patients unwittingly consume multiple NSAIDs through multi-symptom products like Advil PM, Aleve Cold, or Motrin Cold. To avoid these risks, clinical guidance suggests a safer pathway. As noted by medical experts, “Because meloxicam is long-acting, acetaminophen can help control breakthrough pain without raising NSAID risks.” Acetaminophen serves as a compatible partner for meloxicam, provided the total daily intake remains strictly below the 3,000 mg to 4,000 mg threshold. By pivoting toward this non-NSAID approach, patients can effectively manage fluctuations in pain intensity while preserving the therapeutic benefits of their primary prescription regimen.
The ‘Accident’ Protocol: What to Do If You Mistakenly Mixed Meds
Accidental medication stacking has become an increasingly common clinical concern, often driven by the use of multi-symptom ‘PM’ or ‘Cold’ products—such as Advil PM, Aleve Cold, or Motrin Cold—which frequently contain hidden NSAIDs. Understanding the pharmacology of your medications is the first step in prevention; for instance, meloxicam is a long-acting NSAID typically dosed once daily at 7.5 mg to 15 mg, whereas ibuprofen has a short half-life of approximately two hours, necessitating dosing every four to six hours. This pharmacokinetic difference is why a 24-hour washout period is strictly recommended when switching from ibuprofen to meloxicam to avoid hazardous drug overlap. While meloxicam was originally developed as a more COX-2 selective NSAID to mitigate the gastrointestinal risks associated with older agents like aspirin and ibuprofen, stacking these medications still significantly elevates the risk of stomach ulcers, internal bleeding, and acute kidney injury.
If you suspect you have inadvertently mixed medications, vigilance is essential. According to clinical data, in acute NSAID overdose reports, nausea, vomiting, and epigastric discomfort are common and are usually the most prominent symptoms. Should you experience persistent abdominal pain, dark or tarry stools, or a significant decrease in urinary output, seek emergency medical care immediately. For those managing breakthrough pain while on a meloxicam regimen, acetaminophen remains a safer alternative, provided your total intake is strictly monitored to remain under the 3,000 mg to 4,000 mg daily threshold. While ongoing research into topical NSAIDs may eventually offer a future solution for targeting local pain without the systemic risks inherent in oral stacking, current patient safety relies on cautious label reading and open communication with your healthcare provider.
Switching Protocols: How to Safely Transition Between Pain Relievers
When transitioning your pain management strategy, understanding the pharmacokinetics of your medication is essential for safety. Meloxicam was developed as a more COX-2 selective NSAID to reduce the high rate of stomach issues seen with older drugs like aspirin and ibuprofen. However, these medications function differently: while ibuprofen has a short half-life of approximately two hours and requires dosing every four to six hours, meloxicam is a long-acting NSAID typically dosed once daily at 7.5 mg to 15 mg. For those moving from short-acting options to a consistent regimen—which you can explore further in our Meloxicam 101: Your Daily Guide to Steady Joint Relief—the timing of the switch is critical to prevent dangerous drug accumulation.
Stacking NSAIDs significantly increases the risk of severe gastrointestinal bleeding, stomach ulcers, and kidney damage. This is particularly relevant as patients are increasingly using multi-symptom ‘PM’ or ‘Cold’ products like Advil PM, Aleve Cold, or Motrin Cold, which often contain ‘hidden’ NSAIDs that contribute to accidental toxicity. As noted by Ikon Recovery Centers, “If switching medications, never do so without medical guidance. There is a washout period of: 1 day for acetylsalicylic acid and other NSAIDs.” Adhering to this 24-hour washout period when transitioning from ibuprofen to meloxicam ensures that the previous medication has sufficiently cleared your system, preventing an unsafe overlap.
While managing your transition, if you require relief for breakthrough pain, acetaminophen is generally considered safe alongside meloxicam, provided you remain strictly under the daily limit of 3,000 mg to 4,000 mg. As we look toward the future, ongoing research into topical NSAIDs may eventually provide a safer way to target local pain without the systemic risks associated with oral stacking, but for now, disciplined timing remains your primary defense against complications.