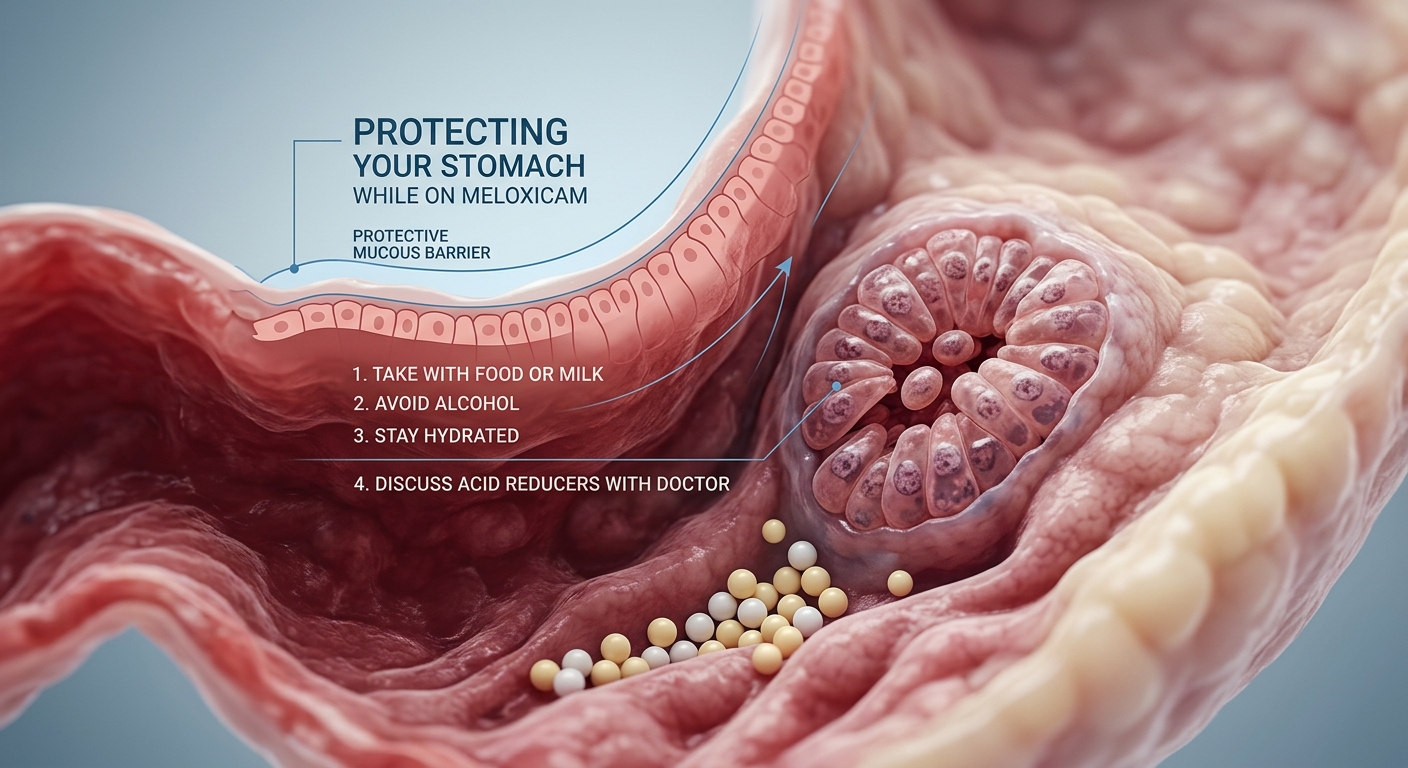
Protecting Your Stomach While on Meloxicam
By Frankie Sze| 5/2/2026
The Stomach-Pain Relief Dilemma
For millions managing chronic arthritis, the pursuit of mobility often feels like a fragile balancing act between systemic relief and internal vulnerability. Historically, clinicians relied on traditional nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or aspirin, yet these legacy options frequently carried a heavy price: a high incidence of debilitating stomach ulcers. The pharmaceutical evolution toward COX-2 selective inhibitors was intended to provide a safer pathway, minimizing the gastric toll while addressing pain. As noted in recent clinical literature, “Both medications reduce inflammation by blocking cyclooxygenase enzymes that produce prostaglandins, the compounds responsible for pain, swelling, and fever.”
Today, meloxicam has emerged as a premier choice for once-daily dosing at 7.5 mg to 15 mg, valued for its convenience and perceived stability. However, the biological reality is more nuanced; while meloxicam is preferentially selective for COX-2, it retains a degree of inhibition over COX-1, which is critical for protecting the gastric mucosa. This duality creates a lingering risk profile where 1.3% to 2.5% of long-term users may face major gastrointestinal complications, such as ulcers or bleeding. For those seeking to navigate this terrain, understanding these risks is essential, a topic we cover in depth in our Meloxicam 101: Your Daily Guide to Steady Joint Relief.
The risk is not uniform. Patients over age 65 face a significantly elevated risk for upper gastrointestinal bleeding (UGIB), and meta-analyses suggest relative risks of 1.24 for meloxicam compared to 1.19 for ibuprofen. Beyond baseline biological risks, patient behaviors—such as the intake of grapefruit juice, which can increase meloxicam blood levels—can exacerbate side effects. While simple adjustments like taking the medication with food can reduce gastric irritation by 40-60%, the future of care is shifting. Clinicians are increasingly looking toward topical NSAIDs to bypass the digestive system entirely or co-prescribing proton-pump inhibitors (PPIs) for high-risk cohorts to ensure that the relief of one joint does not become the detriment of the stomach.
COX-2 Selectivity: Why Meloxicam is Built Differently
For decades, traditional non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and aspirin served as the primary clinical standard for pain management, yet their broad-spectrum inhibition often came at a high cost: significant gastric ulceration. In response, the development of COX-2 selective inhibitors emerged to offer potent pain relief while attempting to minimize the physiological toll on the digestive tract. Meloxicam occupies a unique position in this landscape; as noted in recent literature, “meloxicam is preferentially selective for COX-2 but also inhibits COX-1”. This pharmacological preference allows it to target inflammation-heavy pathways while maintaining a slightly kinder profile to the stomach lining compared to traditional options.
Despite this design, it is essential to recognize that meloxicam is not entirely COX-1 neutral. Meta-analyses reveal relative risks for gastrointestinal complications are approximately 1.19 for ibuprofen compared to 1.24 for meloxicam, underscoring that while the mechanism is refined, the risks persist. Indeed, major GI events such as bleeding or ulcers occur in roughly 1.3% to 2.5% of long-term users, with patients over age 65 facing a significantly elevated risk of upper gastrointestinal bleeding (UGIB). Because of this, clinical best practices now emphasize co-prescribing proton-pump inhibitors (PPIs) for high-risk individuals, alongside recommending that patients take their medication with food, which can reduce gastric irritation by 40-60%. Furthermore, patients should be aware of external factors, such as grapefruit juice, which can increase systemic meloxicam levels and exacerbate side effect risks.
Today, meloxicam remains a leading prescription choice for chronic arthritis, favored for its long-acting profile and once-daily convenience at doses of 7.5 mg to 15 mg. However, as we look toward the future of rheumatology, the clinical focus is shifting—not just toward refining oral agents, but toward the increased utilization of topical NSAIDs, which offer the ability to bypass the digestive system entirely and provide targeted relief without systemic exposure.
The ‘Gentler’ Reality Check: Understanding Residual Risks
Historically, the advent of COX-2 selective inhibitors represented a milestone in rheumatology, promising the potent analgesic benefits of traditional NSAIDs like ibuprofen or aspirin while sparing the gastric mucosa from the high ulcer rates associated with non-selective pathways. Today, meloxicam has solidified its place as a preferred prescription for chronic arthritis, favored for its long-acting profile—typically dosed once daily at 7.5 mg to 15 mg—and its reputation for being a ‘gentler’ alternative. However, it is essential to recognize that meloxicam is only preferentially selective for COX-2; it continues to inhibit COX-1 to a degree that necessitates clinical vigilance.
The statistical reality underscores that this preferential selectivity does not equate to the total absence of risk. A comprehensive medicine review highlights this nuance, noting that in comparative analyses, “meloxicam (RR 1.24; 95% CI 0.98, p=1.56) and ibuprofen had a lower risk (RR 1.19; 95% CI 0.93, p=1.54),” illustrating that the delta between traditional NSAIDs and newer agents is narrower than marketing narratives often suggest. Indeed, major gastrointestinal events, including ulcers and bleeding, manifest in approximately 1.3% to 2.5% of patients during long-term therapy.
For the aging population, particularly those over age 65, the risk of upper gastrointestinal bleeding (UGIB) remains significantly elevated. While taking meloxicam with food can mitigate immediate gastric irritation by 40-60%, patients must also be aware of external factors, such as grapefruit juice, which can increase systemic drug levels and inadvertently heighten the risk of adverse effects. As the medical community moves toward the future—with a growing focus on co-prescribing proton-pump inhibitors (PPIs) and a transition toward topical NSAIDs to bypass the digestive system entirely—patients should view meloxicam as a tool requiring careful management rather than a risk-free necessity.
Red Flags: Distinguishing Upset from Medical Emergencies
While meloxicam was developed to improve upon the gastric profiles of traditional NSAIDs like aspirin and ibuprofen, it remains a potent pharmacological agent. Because meloxicam is preferentially selective for COX-2 but still inhibits COX-1 to some degree, it is not without risk. While taking meloxicam with food can reduce gastric irritation by 40-60%, patients must remain vigilant for signs that a minor side effect has escalated into a medical crisis. Long-term therapy carries a reported 1.3-2.5% risk of major gastrointestinal events, a statistic that demands careful monitoring, especially given that meta-analyses indicate a relative risk of 1.24 for GI complications with meloxicam.
Patients must be particularly aware of their specific risk factors. Those over age 65 face a significantly higher probability of upper gastrointestinal bleeding (UGIB). Furthermore, external factors such as consuming grapefruit juice—which can increase meloxicam levels in the blood—may inadvertently exacerbate side effect risks. As we look toward a future with greater emphasis on co-prescribing proton-pump inhibitors for high-risk users, it is vital that you recognize when to stop medication and seek immediate intervention. According to Ubie Health, you must “seek urgent care for chest pain, shortness of breath, black stools, vomiting blood, severe abdominal pain, or sudden weakness.” These symptoms are not mere stomach upset; they are clinical indicators of potentially life-threatening complications that require an emergency medical response.
Practical Gut-Protection Strategies for Daily Use
While meloxicam is a preferred choice for chronic arthritis due to its once-daily 7.5 mg to 15 mg convenience, its pharmacokinetics demand mindful administration. Because meloxicam is only preferentially selective for COX-2—still inhibiting COX-1 to some degree—it is not entirely devoid of gastrointestinal risk. Studies indicate that major GI events, such as ulcers or bleeding, manifest in approximately 1.3% to 2.5% of long-term users. Clinical data reveals that the relative risk for these complications with meloxicam is 1.24, comparable to the 1.19 observed with ibuprofen. For patients over age 65, these risks are significantly elevated, necessitating heightened vigilance.
The most effective behavioral adjustment is also the simplest: consistency in meal timing. As stated by clinical research, taking meloxicam with food reduces stomach upset by 40-60% according to clinical studies. Pairing your dose with a substantial meal acts as a protective buffer for the gastric mucosa, mitigating the irritation that traditional NSAIDs have long been associated with. Furthermore, patients must be cautious with dietary interactions; specifically, grapefruit juice should be avoided, as it can elevate meloxicam concentrations in the blood, thereby increasing the potential for adverse side effects.
Looking toward the future, the medical community is moving toward co-prescribing proton-pump inhibitors (PPIs) for high-risk individuals and prioritizing topical NSAIDs to bypass the digestive tract entirely. Until such shifts become the universal standard of care, maintaining a strict regimen of taking your medication with food remains the cornerstone of daily gut-protection strategy. Frankie Sze.
When to Consult Your Doctor About GI Safety
While meloxicam is a preferred choice for chronic arthritis due to its once-daily 7.5 mg to 15 mg dosing, patients must remain vigilant regarding gastrointestinal (GI) health. Although the drug is preferentially selective for COX-2, it still inhibits COX-1 to some degree, a trade-off that maintains a relative risk for GI complications similar to traditional NSAIDs like ibuprofen. Data suggests that 1.3% to 2.5% of long-term users experience major events such as ulcers or bleeding, necessitating proactive monitoring.
For patients over age 65, the risk of upper gastrointestinal bleeding (UGIB) is significantly elevated. As clinical standards shift toward greater emphasis on co-prescribing proton-pump inhibitors (PPIs) for these high-risk individuals, consistent medical oversight becomes non-negotiable. As noted by clinical guidelines, providers should “monitor blood counts, renal, and hepatic function… and assess for signs/symptoms of gastrointestinal bleeding.” If you are navigating your treatment, refer back to our Meloxicam 101: Your Daily Guide to Steady Joint Relief for baseline safety protocols.
Patient lifestyle factors also play a critical role in safety. Taking your medication with food can reduce gastric irritation by 40-60%, helping mitigate side effects during daily use. Conversely, be aware of dietary interactions, such as grapefruit juice, which can increase meloxicam levels in the blood and potentially heighten toxicity risks. As the future of pain management moves toward topical NSAIDs that bypass the digestive system entirely, current users should maintain open lines of communication with their healthcare team to ensure that their regimen remains both effective and gentle on the stomach lining.