Can I Take Meloxicam and Ibuprofen Together?
By Frankie Sze | 5/1/2026
The Common Temptation: Why People Want to Mix NSAIDs
When you are grappling with the persistent stiffness of chronic arthritis, the urge to reach for a familiar bottle of ibuprofen alongside your new prescription can feel like the only logical path to relief. As noted by experts, “Patients frequently wonder whether meloxicam or ibuprofen works better for arthritis pain, how quickly each provides relief, and how often they must be taken” [Clinical Pharmacy Insight]. This frustration is understandable; while ibuprofen provides a rapid, albeit fleeting, effect that usually wears off after four to six hours, meloxicam is engineered for steady, long-term management with a long half-life that requires only once-daily dosing. However, doubling down on these medications is a dangerous miscalculation.
Although meloxicam is preferentially selective for COX-2, it still inhibits COX-1, meaning it carries significant ulcer risks similar to its over-the-counter counterparts. Combining two NSAIDs does not double your relief; instead, it compounds your risk of gastrointestinal bleeding by three-fold to seven-fold. To understand why your physician prioritizes the sustained, stable anti-inflammatory coverage of your prescription, it is helpful to review Meloxicam 101: Your Daily Guide to Steady Joint Relief. Transitioning safely between these agents requires strict adherence to timing: if you are switching from ibuprofen to meloxicam, a waiting period of six to ten hours is necessary. Conversely, if you have recently taken meloxicam, you must wait at least 24 hours before considering ibuprofen. Moving forward, the goal of your treatment plan should be finding the lowest effective dose of meloxicam, potentially supplemented by safer non-NSAID adjuncts like acetaminophen, rather than risking your digestive health with overlapping medications.
The ‘Double Trouble’ Rule: A Definitive No
When navigating a pain flare, the temptation to reach for a familiar over-the-counter bottle of ibuprofen while starting a new prescription for meloxicam is understandable, but medically, it is a perilous mistake. As Frankie Sze emphasizes, clinicians offer a clear, definitive stance: “No. These drugs are both NSAIDs and perform similar functions. Therefore, they should not be combined,” according to Ikon Recovery Centers. Far from providing extra relief, taking these medications together is redundant and increases the risk of gastrointestinal bleeding by 3-fold to 7-fold.
The pharmacological profiles of these agents highlight why they cannot be safely layered. Ibuprofen is a short-acting agent with effects generally wearing off after 4 to 6 hours, whereas meloxicam is a once-daily medication with a significantly longer half-life. Because meloxicam is preferentially selective for COX-2 but still inhibits COX-1, it continues to carry intrinsic ulcer risks that are compounded by the addition of other NSAIDs. To ensure patient safety, strict temporal boundaries are required: a waiting period of 6 to 10 hours is advised when switching from ibuprofen to meloxicam, while a much longer interval of at least 24 hours must pass after taking meloxicam before the use of ibuprofen can be considered. Moving forward, your long-term management strategy should prioritize the lowest effective dose of meloxicam and the integration of non-NSAID adjuncts, such as acetaminophen, rather than doubling down on systemic anti-inflammatory risks.
Mechanism of Risk: How Stacking Blocks Vital Organs
When you take an anti-inflammatory medication, you are engaging a potent biological feedback loop. As noted by Doctronic, “Both medications reduce inflammation by blocking cyclooxygenase enzymes that produce prostaglandins, the compounds responsible for pain, swelling, and fever.” While this inhibition effectively targets your discomfort, these same prostaglandins serve a critical, protective role in your body: they maintain the integrity of your stomach lining and regulate blood flow to your kidneys. When you combine medications—a common scenario for patients transitioning from over-the-counter ibuprofen for acute pain to a prescribed regimen of meloxicam for chronic arthritis—you risk stripping away these vital defenses entirely.
The biological danger stems from the distinct pharmacokinetic profiles of these two drugs. Ibuprofen is short-acting, with effects generally wearing off after 4 to 6 hours, whereas meloxicam possesses a long half-life, allowing for once-daily dosing at 7.5 mg to 15 mg. Although meloxicam is preferentially selective for COX-2, it still inhibits COX-1, meaning it inherently carries ulcer risks similar to other NSAIDs. Stacking these agents creates a compounding effect that can increase the risk of gastrointestinal bleeding by 3-fold to 7-fold. For those navigating a pain flare, the temptation to reach for an old bottle of ibuprofen while on meloxicam is high, but the clinical reality demands caution: a waiting period of 6 to 10 hours is recommended when switching from ibuprofen to meloxicam, and if you have already taken meloxicam, a period of at least 24 hours is required before safely introducing ibuprofen. Moving forward, sustainable pain management should prioritize the lowest effective dose of meloxicam alongside non-NSAID adjuncts like acetaminophen to preserve long-term organ health.
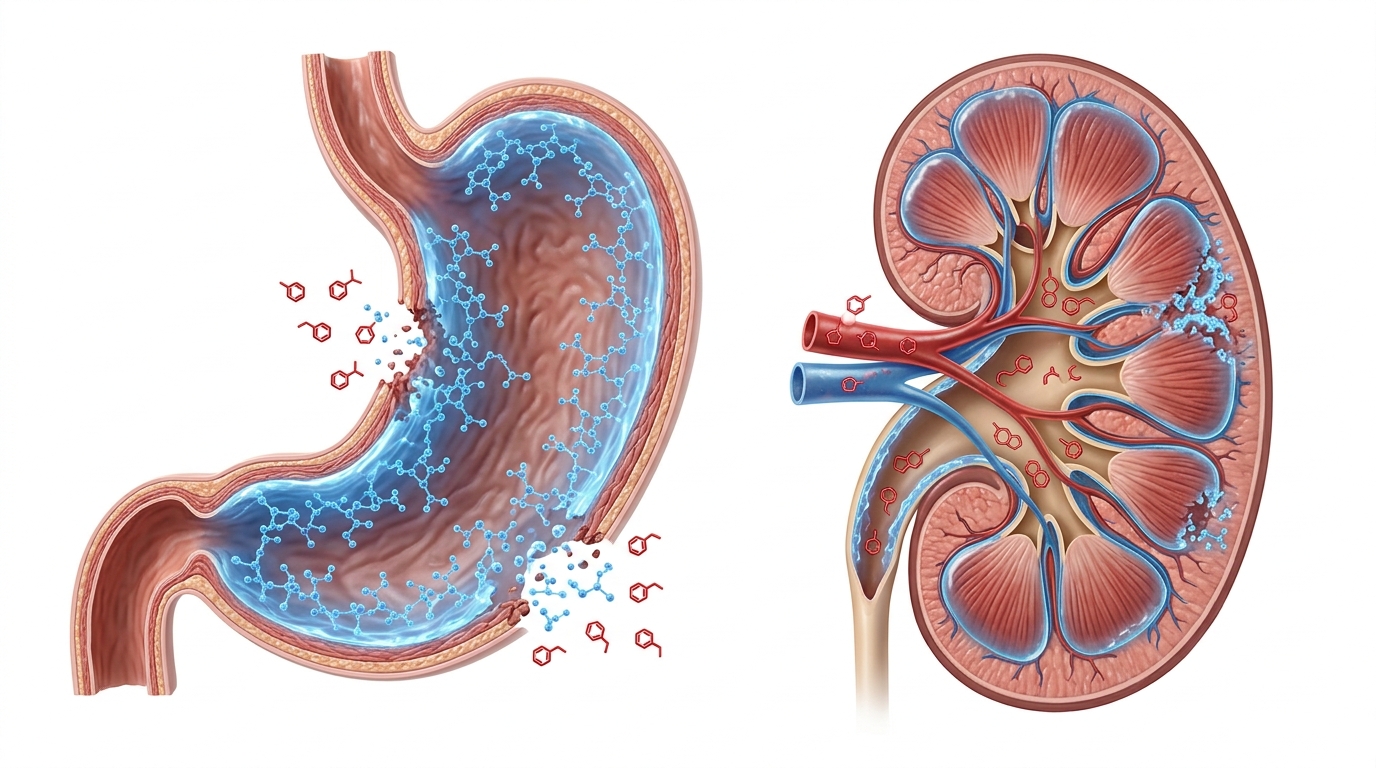
Major Health Hazards: GI Bleeds, Kidney Stress, and Heart Risk
When patients transition from over-the-counter ibuprofen for acute discomfort to a prescribed regimen of meloxicam for chronic arthritis, the temptation to stack these therapies during a pain flare is both common and perilous. However, clinical evidence highlights that combining these agents creates a dangerous synergistic effect. As noted by industry experts, “Because both medications are NSAIDs, taking them together increases the risk of side effects, such as stomach ulcers, gastrointestinal bleeding, or kidney damage.”
The quantitative reality of this danger is stark: dual-NSAID therapy is associated with a 3-fold to 7-fold increase in the risk of serious gastrointestinal bleeding. While meloxicam is preferentially selective for COX-2, it retains enough COX-1 inhibition to maintain significant ulcerogenic potential. Furthermore, the pharmacokinetics of these drugs necessitate strict temporal boundaries that patients often overlook. Ibuprofen is a short-acting agent with effects typically waning after 4 to 6 hours, whereas meloxicam possesses a long half-life, requiring only once-daily dosing of 7.5 mg to 15 mg. Due to this long-acting profile, a waiting period of at least 24 hours is required after a meloxicam dose before introducing ibuprofen; conversely, a buffer of 6 to 10 hours is recommended when switching from ibuprofen to meloxicam.
For those managing chronic pain, the goal of long-term care must remain the use of the lowest effective dose of meloxicam, potentially supplemented by non-NSAID adjuncts like acetaminophen, rather than risking the severe renal and cardiovascular complications inherent in poly-NSAID use.
Accidental Overlap: What to Do if You Took Both
When managing pain, it is common to start with over-the-counter ibuprofen for minor aches before moving to a prescribed regimen of meloxicam for chronic conditions. However, accidental overlap is a serious concern. Because dual NSAID therapy can increase the risk of gastrointestinal bleeding by three-fold to seven-fold, strict adherence to timing is essential. While ibuprofen effects typically wear off after four to six hours, meloxicam has a significantly longer half-life and is dosed once daily at 7.5 mg to 15 mg. Because meloxicam is preferentially selective for COX-2 but still inhibits COX-1, it carries inherent ulcer risks that are compounded when combined with other NSAIDs.
If you are switching medications, a waiting period of 6 to 10 hours is required when moving from ibuprofen to meloxicam; however, if you have already taken meloxicam, you must wait at least 24 hours before introducing ibuprofen. Should an accidental ingestion occur, remain vigilant for symptoms such as severe abdominal pain, black or tarry stools, or vomiting blood. As noted by New Waters Recovery, “An NSAID overdose is a medical emergency. If you suspect someone overdosed on an NSAID like meloxicam or ibuprofen, call 911.” If symptoms are mild, contact your primary care physician or poison control immediately to determine the next steps in your care.
Managing Breakthrough Pain: Safer Alternatives to Ibuprofen
When you are grappling with a chronic arthritis flare, the temptation to reach for a familiar bottle of over-the-counter ibuprofen is understandable, especially if your prescribed meloxicam has not yet provided complete relief. However, combining these two medications is clinically discouraged. While meloxicam is preferentially selective for COX-2, it still retains enough COX-1 inhibition to carry significant ulcer risks. Compounding this with ibuprofen—which only provides relief for 4 to 6 hours—is dangerous; dual NSAID therapy can increase the risk of gastrointestinal bleeding by 3-fold to 7-fold. Because meloxicam possesses a long half-life and is typically dosed once daily (7.5 mg to 15 mg), the body requires a waiting period of at least 24 hours after a meloxicam dose before introducing ibuprofen, or a 6 to 10-hour window when switching in the reverse direction.
Instead of risking these stacking effects, many clinicians recommend a non-NSAID adjunct to manage breakthrough pain. As noted by clinical experts, “Yes, you can generally take meloxicam and Tylenol (acetaminophen) together safely. These medications work through different mechanisms and don’t typically interact with each other.” By utilizing acetaminophen as a partner to your meloxicam, you can address pain through a different biological pathway without elevating the risk of gastric injury. Long-term management should always focus on maintaining the lowest effective dose of meloxicam, supplementing only with safer, non-NSAID alternatives when symptoms escalate.
Expert Guidance: When to Adjust Your Meloxicam Prescription
When navigating chronic arthritis, it is common to have a history of relying on over-the-counter ibuprofen for minor aches before transitioning to a prescription-strength regimen like meloxicam. However, if you are experiencing a pain flare, the instinct to supplement your current prescription with leftover ibuprofen is medically hazardous. As noted in clinical research, “It is administered as an oral dose of 7.5 mg, which can be increased if necessary, to a maximum of 15 mg per day.” Rather than risking the complications of dual therapy, which can increase the risk of gastrointestinal bleeding by 3-fold to 7-fold, you should always consult your physician to discuss potential dosage adjustments within this safe therapeutic window.
Understanding the pharmacology of these medications is vital for your safety. While ibuprofen effects typically wear off after 4 to 6 hours, meloxicam features a significantly longer half-life, necessitating only once-daily dosing. Because meloxicam is preferentially selective for COX-2 but still inhibits COX-1, it carries inherent ulcer risks that are compounded by the addition of other NSAIDs. For those transitioning between medications, a strict waiting period of 6 to 10 hours is recommended when moving from ibuprofen to meloxicam, while a waiting period of at least 24 hours is required after taking meloxicam before introducing ibuprofen. For more foundational information on maintaining consistent therapeutic levels, please review our guide on Meloxicam 101: Your Daily Guide to Steady Joint Relief.
Ultimately, long-term management should focus on identifying the lowest effective dose of meloxicam under professional supervision rather than self-medicating. If your current dose is insufficient, your healthcare provider may suggest non-NSAID adjuncts, such as acetaminophen, to manage breakthrough pain safely. Prioritizing this collaborative approach with your clinician ensures your treatment remains effective while minimizing the risks associated with polypharmacy. — Frankie Sze