Meloxicam vs. Ibuprofen: Which is Stronger?
By Frankie Sze | 5/1/2026
Introduction: The ‘Strength’ Misconception in Pain Relief
When patients approach their healthcare providers with questions about chronic inflammation and joint pain, one of the most common inquiries centers on potency. As clinicians, we often hear: “Patients frequently wonder whether meloxicam or ibuprofen works better for arthritis pain, how quickly each provides relief, and how often they must be taken,” notes a recent clinical analysis on NSAID management. Yet, the search for the “strongest” medication often misses the nuanced reality of how these drugs function within the body.
The misconception of strength usually ignores the distinction between speed and endurance. Ibuprofen, long the gold standard for over-the-counter pain management, is designed for rapid onset; it typically begins working within 20–30 minutes. In contrast, meloxicam is significantly more potent—10 to 20 times more so than ibuprofen on a milligram-for-milligram basis—but it functions on a different timeline. While a 15 mg dose of meloxicam is clinically equivalent to 1,200–2,400 mg of daily ibuprofen for treating rheumatoid arthritis, it requires about one hour for initial relief and hits its peak effect only after 5 to 6 hours. For those looking to understand these mechanics further, our Meloxicam 101: Your Daily Guide to Steady Joint Relief provides a comprehensive breakdown of how these profiles align with different pain types.
This shift from acute, rapid-response pain relief to chronic, maintenance-based therapy defines the 2025-2026 clinical landscape. While ibuprofen remains a staple for short-term injury, its 4–6 hour duration often creates gaps in coverage for chronic sufferers. Meloxicam provides a 24-hour therapeutic window with a single dose, naturally boosting patient adherence rates to 70-80%, compared to the 50-60% observed with multi-dose ibuprofen regimens. However, as we look toward future developments in COX-2 selectivity aimed at mitigating gastrointestinal risks, patients must remember that these medications are not interchangeable; combining them is strictly unsafe due to the compounding risks of ulcers and kidney damage. Furthermore, both agents necessitate caution—particularly after the 20th week of pregnancy—reminding us that the “best” medication is not merely the strongest, but the one most precisely matched to the duration and nature of the underlying condition.
Potency vs. Persistence: Defining What ‘Stronger’ Really Means
When patients inquire whether meloxicam is ‘stronger’ than ibuprofen, the answer requires distinguishing between chemical potency and pharmacological duration. As clinical research indicates, meloxicam is 10 to 20 times more potent than ibuprofen on a milligram-for-milligram basis. This structural efficiency means that a standard 15 mg dose of meloxicam is clinically comparable to taking between 1,200 mg and 2,400 mg of ibuprofen over the course of a day to manage conditions like rheumatoid arthritis.
However, strength also encompasses temporal reach. Ibuprofen is designed for rapid onset, typically providing relief within 20–30 minutes, though its effects wane quickly, requiring repeated dosing every 4–6 hours. In contrast, meloxicam is a ‘long-game’ medication; while it takes roughly one hour to provide initial relief and up to six hours to reach peak effect, it offers stable, 24-hour coverage with a single daily dose. This pharmacokinetic difference directly influences patient outcomes: adherence rates for once-daily meloxicam sit at 70–80%, significantly higher than the 50–60% observed with the multi-dose regimen required by ibuprofen. While both medications remain essential tools in pain management, clinicians are increasingly emphasizing the need to match a drug’s half-life to the nature of the patient’s discomfort, selecting rapid-acting options for acute spikes and persistent formulations for chronic management.
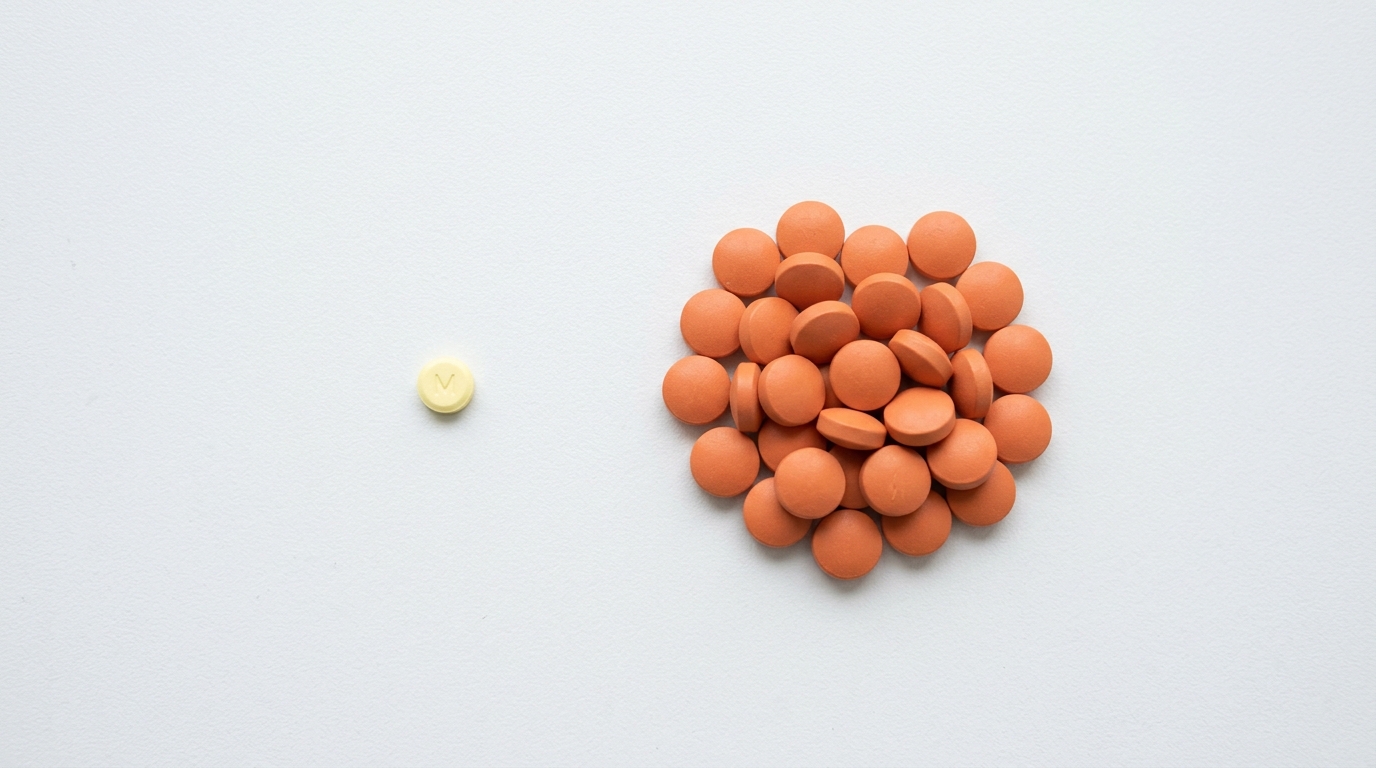
Speed vs. Stamina: Comparing Onset Times and Half-Life
When selecting an NSAID, clinicians must evaluate the specific temporal needs of the patient’s condition. Ibuprofen serves as the quintessential ‘sprinter’ of pain management; as noted in recent clinical literature, “Ibuprofen is characterized as a short-acting Nonsteroidal Anti-inflammatory Drug (NSAID)… providing noticeable relief within 20 to 30 minutes. However, this quick sprint comes at a cost: ibuprofen has a short half-life,” typically lasting only 4–6 hours. This necessitates frequent dosing to maintain therapeutic blood levels, which often correlates with lower adherence rates of 50-60%.
In contrast, meloxicam functions as the ‘marathon’ runner of the pharmacological world. While it requires roughly one hour for initial relief and reaches peak effect between 5–6 hours, its true value lies in its 24-hour coverage. Meloxicam is significantly more potent—10 to 20 times more so than ibuprofen on a milligram-for-milligram basis—allowing a single 15 mg dose to provide clinical outcomes comparable to 1,200–2,400 mg of daily ibuprofen for rheumatoid arthritis patients. This convenience significantly improves patient outcomes, with adherence rates reaching 70-80% for once-daily regimens.
While generic meloxicam is more expensive at $25–$45 per 30-day supply compared to $7–$10 for OTC ibuprofen, the clinical decision often hinges on the distinction between acute relief and chronic maintenance. Regardless of the choice, safety remains paramount: both medications are contraindicated after the 20th week of pregnancy due to risks of reduced amniotic fluid, and patients must never combine these agents, as the dual-administration drastically increases the risk of gastrointestinal ulcers and renal impairment.

Clinical Use Cases: Chronic Inflammation vs. Acute Pain Episodes
Choosing between meloxicam and ibuprofen requires a precise alignment of the medication’s pharmacokinetics with the nature of the patient’s discomfort. While ibuprofen has long served as the standard for acute, episodic pain management, meloxicam was engineered to address the specific needs of patients suffering from chronic inflammation. As noted by Drugs.com, “Meloxicam is only approved to treat pain or inflammation caused by arthritis… Ibuprofen is FDA approved to treat most mild-to-moderate painful conditions, such as toothache, back pain, and primary dysmenorrhea.”
The temporal dynamics of these two agents differ significantly, impacting their clinical application. Ibuprofen offers rapid onset, typically beginning to alleviate pain within 20–30 minutes, though its effects persist for only 4–6 hours. In contrast, meloxicam requires approximately one hour for initial relief, with peak effects reached between 5–6 hours. Despite this slower start, meloxicam provides 24-hour coverage with a single dose. This dosing convenience contributes to improved patient adherence, which averages 70–80% for once-daily meloxicam compared to 50–60% for multi-dose regimens required by ibuprofen.
On a milligram-for-milligram basis, meloxicam exhibits 10 to 20 times the potency of ibuprofen. Clinically, a 15 mg dose of meloxicam is comparable to 1,200–2,400 mg of daily ibuprofen for rheumatoid arthritis management. While the economic accessibility of OTC ibuprofen ($7–$10) versus generic meloxicam ($25–$45 for a 30-day supply) is a factor in selection, safety remains paramount. Combining these two NSAIDs is strictly contraindicated, as the synergy significantly elevates risks of renal impairment and gastric ulceration. Furthermore, clinical vigilance is required for all patients of childbearing age; both medications must be avoided after the 20th week of pregnancy due to the risk of reduced amniotic fluid levels.
Dosing Convenience: The Impact of Once-Daily vs. Multi-Dose Routines
For patients managing chronic conditions like rheumatoid arthritis, the burden of a multi-dose medication schedule is a significant barrier to effective pain management. While ibuprofen has long served as a standard over-the-counter analgesic, its 4–6 hour half-life often necessitates frequent dosing, which increases the likelihood of ‘breakthrough pain’ as blood concentrations wane. In contrast, meloxicam offers a pharmacokinetically superior alternative for long-term care. Although ibuprofen acts faster—providing initial relief within 20–30 minutes compared to meloxicam’s one-hour onset—the latter is 10 to 20 times more potent on a milligram-for-milligram basis. A 15 mg dose of meloxicam provides 24-hour therapeutic coverage, effectively replacing the 1,200–2,400 mg of ibuprofen that would otherwise be required daily.
The impact of this clinical difference on patient behavior is profound. Research indicates that adherence rates for once-daily meloxicam reach 70–80%, significantly higher than the 50–60% observed with multi-dose ibuprofen regimens. As noted by experts at The Freedom Center, “With a single pill taken per day, rather than needing to remember to take multiple doses at different times, patients have a better chance of adhering to their medication schedule.” While the cost remains a consideration—with generic meloxicam ranging from $25–$45 per month compared to $7–$10 for over-the-counter ibuprofen—the clinical benefit of consistent, steady-state relief often outweighs the economic disparity for those with chronic inflammatory markers.
As we navigate current 2025–2026 guidelines, clinicians are increasingly encouraged to align NSAID selection with the temporal nature of a patient’s pain. However, caution remains paramount: patients must never combine these agents, as the risk of gastrointestinal ulceration and renal impairment rises sharply with polypharmacy. Furthermore, both medications must be avoided after the 20th week of pregnancy due to the risk of oligohydramnios. By choosing the dosing frequency that best matches the patient’s lifestyle, we can improve long-term outcomes while minimizing the fluctuations that lead to uncontrolled pain.
Safety Profiles: COX-2 Selectivity and Gastrointestinal Tolerability
A critical differentiator in the clinical utility of meloxicam lies in its pharmacological selectivity. While traditional non-selective NSAIDs like ibuprofen inhibit both COX-1 and COX-2 enzymes—the latter of which is responsible for maintaining the protective gastric lining—meloxicam exhibits a greater affinity for inhibiting COX-2. As noted in clinical perspectives, “Meloxicam targets the COX-2 enzyme, reducing inflammation and pain with fewer stomach side effects than many traditional NSAIDs” (AMSK Insights).
This selectivity offers a distinct advantage for patients requiring long-term management of chronic conditions. Although ibuprofen remains the gold standard for acute, short-term relief due to its rapid onset of 20–30 minutes, it requires frequent dosing every 4–6 hours, which can complicate adherence. In contrast, meloxicam’s pharmacokinetics provide 24-hour coverage with a single dose; while it takes approximately one hour for initial relief and 5–6 hours for peak effect, its consistent duration facilitates much higher patient adherence rates of 70–80%, compared to the 50–60% often seen with multi-dose regimens. Clinicians are increasingly matching these profiles to patient needs, noting that a 15 mg dose of meloxicam—which is 10 to 20 times more potent than ibuprofen on a milligram-for-milligram basis—is clinically comparable to a daily total of 1,200–2,400 mg of ibuprofen for rheumatoid arthritis.
Despite these benefits, safety remains paramount. While generic meloxicam is more costly at $25–$45 per 30-day supply compared to $7–$10 for OTC ibuprofen, the economic value is secondary to clinical safety. Both medications carry significant risks, including the necessity to avoid use after the 20th week of pregnancy due to potential impacts on amniotic fluid levels. Furthermore, patients must never combine these two agents, as dual administration significantly heightens the risk of gastrointestinal ulceration and renal damage. As research continues into the future of NSAID therapy, the focus remains on refining this balance of efficacy and gastrointestinal tolerability.
Verdict: Choosing the Right Tool for Your Specific Pain
When navigating the landscape of nonsteroidal anti-inflammatory drugs, the decision hinges on the nature of your discomfort. As noted by Doctronic AI, “Your choice depends on whether you need sustained relief for ongoing inflammation or quick action for sudden pain episodes.” Ibuprofen remains the gold standard for acute, short-term needs, as it begins working in just 20–30 minutes. However, its effectiveness is fleeting, necessitating repeat dosing every 4–6 hours.
Conversely, meloxicam represents a more potent, specialized tool for those managing chronic conditions like rheumatoid arthritis. On a milligram-for-milligram basis, meloxicam is 10 to 20 times more potent than ibuprofen; a single 15 mg dose is clinically equivalent to 1,200–2,400 mg of daily ibuprofen. While it takes roughly one hour for initial relief and up to six hours for peak effect, its 24-hour coverage makes it superior for persistent joint inflammation. This convenience translates to higher patient adherence, with rates of 70–80% for once-daily meloxicam compared to 50–60% for multi-dose regimens. For more on optimizing your long-term management, see Meloxicam 101: Your Daily Guide to Steady Joint Relief.
From a financial perspective, generic meloxicam currently costs between $25–$45 for a 30-day supply, whereas over-the-counter ibuprofen is more accessible at $7–$10. Regardless of your choice, clinical vigilance is mandatory. Both medications must be avoided after the 20th week of pregnancy due to risks of reduced amniotic fluid, and they should never be combined, as doing so significantly elevates the risk of kidney damage and stomach ulcers. As we look toward future developments in COX-2 selectivity, the goal remains to tailor therapy to your specific pain duration while minimizing systemic risks.



