Meloxicam vs. Ibuprofen: Choosing Between Chronic and Acute Relief
By Frankie Sze | 5/2/2026
Introduction: Understanding the NSAID Spectrum
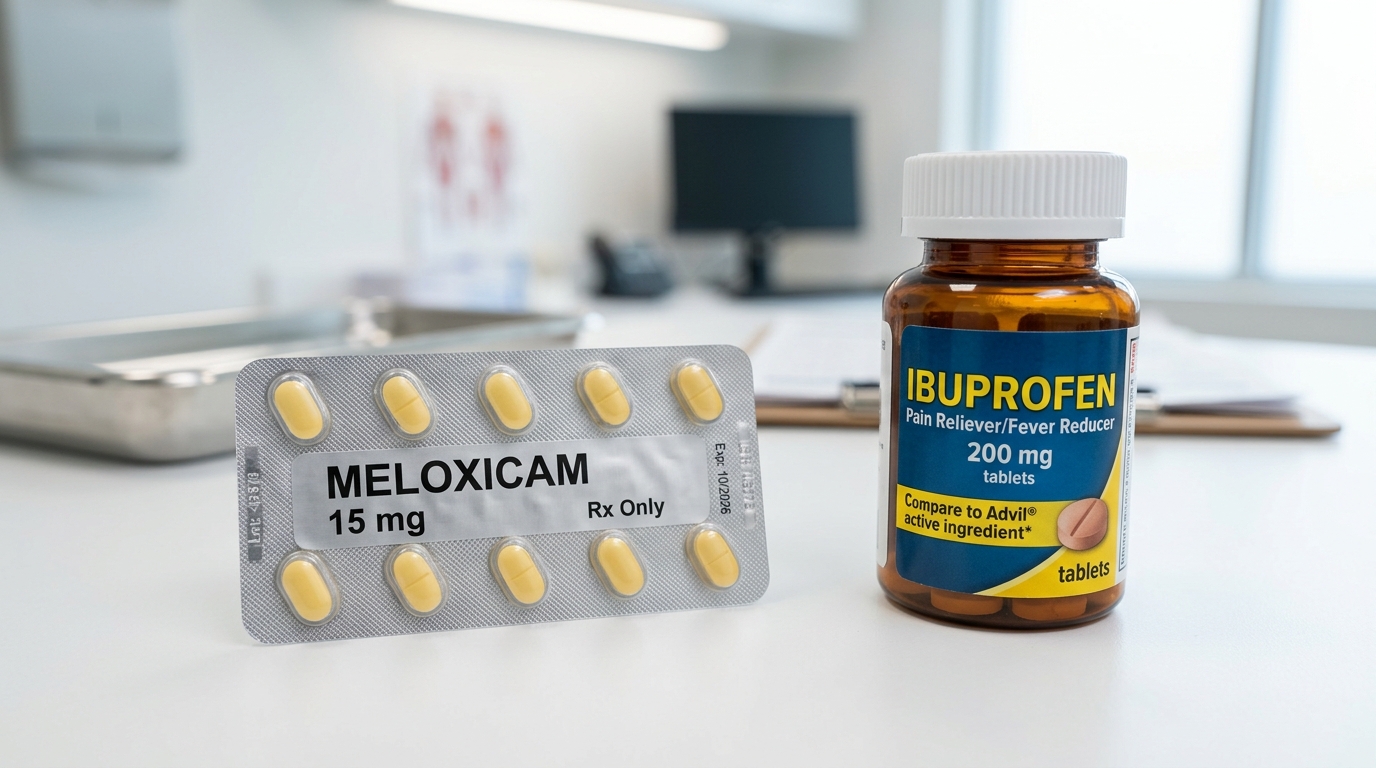
While both meloxicam and ibuprofen fall under the broader umbrella of nonsteroidal anti-inflammatory drugs (NSAIDs), they are far from interchangeable. As noted by The Freedom Center, “Meloxicam and ibuprofen are both NSAIDs that reduce pain and inflammation, but meloxicam is prescription-only while ibuprofen is available over-the-counter.” Historically, the development of COX-2 selective agents was intended to mitigate the significant gastrointestinal complications frequently associated with traditional, non-selective NSAIDs like ibuprofen. Today, we understand that these medications serve distinct strategic roles based on their pharmacokinetic profiles.
For patients managing chronic conditions like arthritis, meloxicam has become a first-line clinical choice in 2026. Because meloxicam is preferentially selective for COX-2—though it does inhibit COX-1 at higher doses—and possesses a terminal elimination half-life of 15 to 20 hours, it offers the convenience of once-daily dosing. However, reaching therapeutic efficacy requires patience, as steady-state concentrations are typically achieved only after 3 to 5 days. For those interested in the logistics of this regimen, Meloxicam 101: Your Daily Guide to Steady Joint Relief provides a comprehensive look at optimizing this therapy. In contrast, ibuprofen provides rapid relief, often within 30 to 60 minutes of ingestion; however, because its effects dissipate within 4 to 6 hours, it necessitates frequent dosing that is rarely practical for chronic, long-term inflammation.
Economic accessibility remains a factor, with generic 15 mg meloxicam tablets retailing between $25 and $45 for a 30-day supply in 2026. Despite these differences, clinicians must emphasize caution: combining these two agents is strictly contraindicated, as the therapeutic overlap significantly increases the risk of gastric ulceration and acute kidney injury. Furthermore, all NSAIDs require careful management in specific populations, particularly regarding cardiovascular health in aging cohorts and pregnancy, where they should be avoided at or after 20 weeks of gestation.
The Meloxicam Strategy: Steady-State Control for Chronic Arthritis
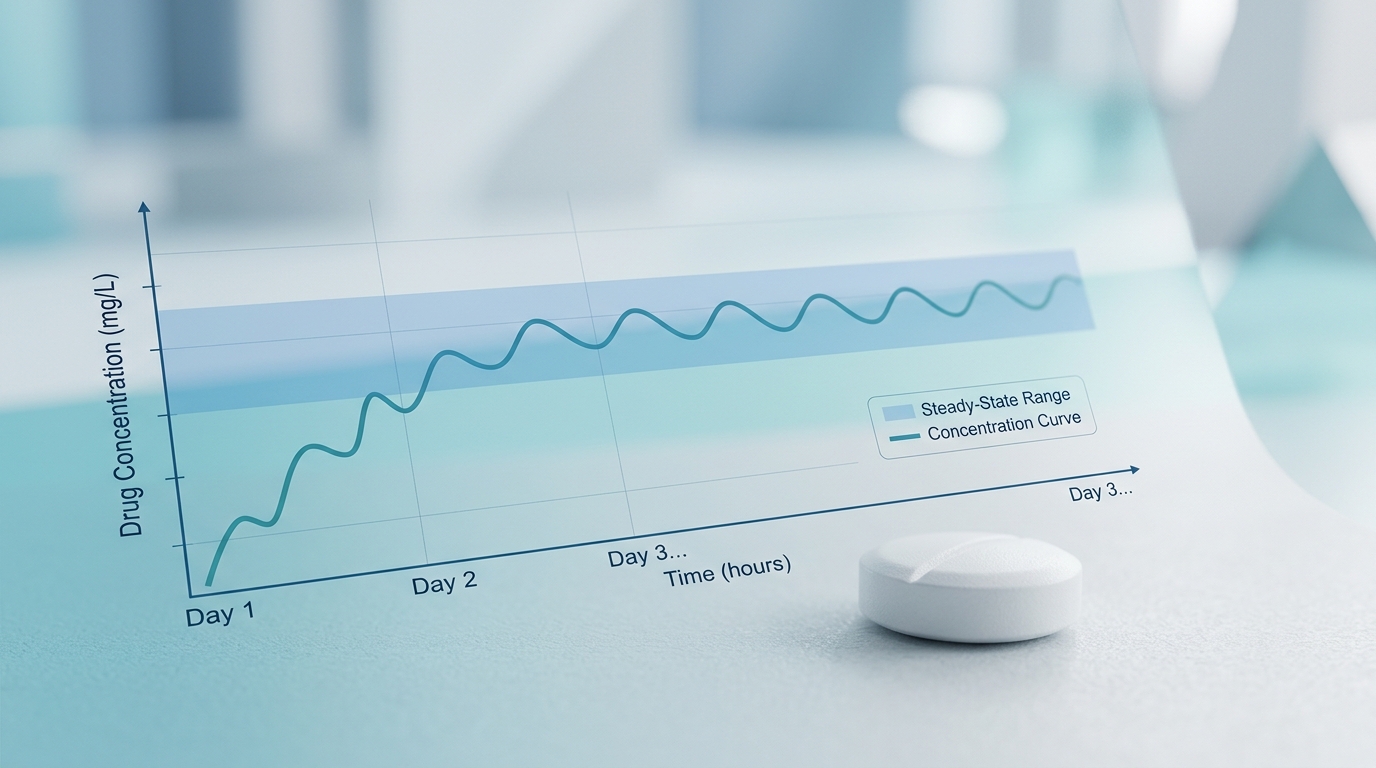
In the landscape of chronic pain management, therapeutic duration is as critical as potency. While traditional non-selective NSAIDs like ibuprofen offer rapid, short-term relief—typically taking effect within 30 to 60 minutes but wearing off after just 4 to 6 hours—they necessitate frequent, inconvenient dosing schedules that can disrupt the lives of those managing long-term inflammatory conditions. In contrast, meloxicam functions as the ‘marathon runner’ of pain relief. With a terminal elimination half-life of 15 to 20 hours, it provides sustained therapeutic coverage that shifts the focus from reactive symptom management to consistent, steady-state control.
As noted by experts in pain management, “Meloxicam offers once-daily dosing with longer-lasting effects, making it preferred for chronic inflammatory conditions like arthritis.” By maintaining a stable serum concentration, which is typically reached after 3 to 5 days of once-daily administration, meloxicam allows for a consistent suppression of inflammation. This mechanism is rooted in its preferential selectivity for the COX-2 enzyme, an evolution in pharmacology designed to mitigate the high rate of gastrointestinal complications common with older, non-selective NSAIDs, though it is important to note that it still inhibits COX-1 at higher dosages. As of 2026, its accessibility remains a significant clinical advantage, with generic 15 mg tablets generally retailing between $25 and $45 for a 30-day supply, solidifying its place as a first-line, cost-effective choice for sustained care.
While this steady-state strategy offers significant benefits, it demands clinical caution. Patients must be advised that combining meloxicam with ibuprofen is strictly contraindicated, as the synergy of these agents exponentially increases the risk of severe stomach ulcers and kidney damage. Furthermore, as guidelines continue to evolve regarding long-term cardiovascular safety in aging populations, practitioners must remain vigilant. Finally, all patients of childbearing age must be informed that NSAIDs should be avoided at or after 20 weeks of pregnancy due to risks of fetal renal impairment.
The Ibuprofen Role: Rapid Response for Acute Flares
While meloxicam serves as a long-term anchor for chronic arthritis management due to its once-daily convenience, ibuprofen acts as the clinical ‘sprinter’ when patients experience sudden, acute flares. Because ibuprofen typically provides relief within 30-60 minutes of ingestion, it is often the preferred tool for immediate intervention. As noted by The Freedom Center, “Ibuprofen works quickly for acute pain relief but requires multiple doses throughout the day for sustained effect.” Its short duration of action—lasting only 4-6 hours—highlights the necessity of frequent dosing, which distinguishes it from the steady-state efficacy profile of meloxicam.
Clinicians must emphasize that despite their shared classification as NSAIDs, these medications serve fundamentally different purposes. Patients must be strictly cautioned against combining these two agents. Concurrent use is contraindicated due to a significantly elevated risk of serious side effects, including gastrointestinal ulcers and acute kidney injury. Furthermore, regardless of the choice between a long-acting prescription like meloxicam or an over-the-counter option, all NSAIDs must be avoided by women at 20 weeks of pregnancy or later to prevent potential fetal complications. Understanding this distinction is vital for patient safety, as the therapeutic goals for managing persistent inflammation differ vastly from the need for rapid, reactive pain control.

Head-to-Head: Onset vs. Duration for Joint Stiffness
When managing the chronic burden of joint stiffness, the therapeutic timeline dictates the clinical approach. For patients seeking rapid, acute intervention, traditional non-selective NSAIDs remain the gold standard; as noted by The Freedom Center, “You’ll typically feel relief within 30-60 minutes.” Ibuprofen serves this purpose well, though its efficacy is ephemeral, lasting only 4-6 hours and necessitating frequent, multi-dose regimens throughout the day. This creates a cycle of peak-and-trough blood levels that can be burdensome for those with persistent mobility issues.
In contrast, meloxicam offers a starkly different pharmacokinetic profile. By being preferentially selective for COX-2—though it does inhibit COX-1 at higher doses—it was developed to mitigate the gastrointestinal complications often associated with older agents like ibuprofen. However, this clinical benefit requires patience: meloxicam has a terminal elimination half-life of 15-20 hours, and steady-state concentrations are not achieved until 3-5 days of consistent, once-daily dosing. While it lacks the rapid ‘rescue’ capability of ibuprofen, its convenience and affordability—with 2026 generic pricing often ranging from $25 to $45 for a 30-day supply—make it a preferred long-term maintenance therapy.
Patients and providers alike must exercise caution, however. Combining meloxicam and ibuprofen is strictly contraindicated, as the cumulative pharmacological load significantly elevates the risk of gastric ulceration and nephrotoxicity. Furthermore, safety mandates require that all NSAIDs be avoided in patients at or beyond 20 weeks of pregnancy. As we look toward future clinical guidelines, the balance between meloxicam’s once-daily convenience and the potential for long-term cardiovascular risks remains a critical focus for practitioners supporting an aging demographic.
Safety Profiles: COX-2 Selectivity and Long-term Organ Health
The pharmacological evolution of nonsteroidal anti-inflammatory drugs (NSAIDs) has been defined by the pursuit of targeted enzyme inhibition. Traditional, non-selective agents like ibuprofen provide rapid relief within 30-60 minutes, though their short 4-6 hour duration of effect necessitates frequent daily dosing for chronic pain management. In contrast, meloxicam offers the convenience of once-daily administration, reaching steady-state concentrations after 3-5 days due to its terminal elimination half-life of 15-20 hours. While meloxicam is preferentially selective for COX-2, clinical data confirms that it also inhibits COX-1 at higher doses, a nuance that informs its therapeutic profile. As noted by Doctronic experts, “meloxicam’s selectivity may reduce stomach irritation compared to ibuprofen, though both medications still carry gastrointestinal risks with long-term use.”
Despite the development of COX-2 selective agents aimed at reducing gastrointestinal complications, the clinical reality for patients in 2026 remains complex. Patients often opt for the cost-effectiveness of generics, with 30-tablet supplies of 15 mg meloxicam ranging from $25 to $45. However, accessibility does not mitigate systemic risk. Combining meloxicam and ibuprofen is strictly contraindicated, as the cumulative pharmacological load significantly elevates the risk of gastric ulceration and acute kidney injury. Furthermore, cardiovascular safety remains a primary concern for aging populations; clinicians must remain vigilant regarding the potential for heart-related adverse events associated with all NSAIDs. In addition to renal and cardiovascular surveillance, practitioners must advise that NSAIDs be avoided in patients who are 20 weeks or further into pregnancy to prevent potential fetal complications. Ongoing monitoring remains essential to balance the symptomatic benefits of chronic pain management against the inevitable risks to long-term organ health.
Practical Realities: Prescription Barriers and 2026 Cost Comparison
For patients managing chronic arthritis, the logistical divide between over-the-counter options and prescription therapies remains a defining aspect of clinical care. Ibuprofen, a traditional non-selective NSAID, offers rapid relief within 30 to 60 minutes; however, its short half-life necessitates multiple daily doses, which can be burdensome for those requiring long-term management. Conversely, meloxicam has been designed for once-daily convenience, reaching steady-state concentrations after only 3 to 5 days of consistent dosing thanks to its terminal elimination half-life of 15 to 20 hours. While the historical development of COX-2 selective NSAIDs sought to mitigate the gastrointestinal complications prevalent with ibuprofen, it is crucial to note that meloxicam remains preferentially selective for COX-2 only at lower doses, inhibiting COX-1 as dosages increase.
In 2026, the economic landscape reflects a shift toward accessible generic maintenance therapy. As noted by clinical data, the retail price for a 30‑tablet supply of generic meloxicam 15 mg ranges from roughly $25 to $45. Despite this affordability, the barrier of a required physician consultation persists, which serves as a necessary safety checkpoint. Because combining meloxicam and ibuprofen is strictly contraindicated due to the heightened risk of stomach ulcers and renal impairment, professional oversight is essential. Furthermore, clinicians must weigh long-term cardiovascular risks—which continue to shape 2026 guidelines—against the immediate therapeutic need, while maintaining vigilance regarding absolute contraindications, such as the avoidance of all NSAIDs at 20 weeks gestation or later.
Conclusion: Matching the Medication to Your Pain Profile
Determining the ideal non-steroidal anti-inflammatory drug (NSAID) requires a clinical assessment of your specific pain profile. As noted in expert guidance, “Your choice depends on whether you need sustained relief for ongoing inflammation or quick action for sudden pain episodes.” For chronic conditions like arthritis, the pharmacokinetic profile of meloxicam—specifically its terminal elimination half-life of 15–20 hours—allows for once-daily dosing. With steady-state concentrations reached after 3–5 days, this medication provides the consistent coverage many patients require, as detailed further in Meloxicam 101: Your Daily Guide to Steady Joint Relief. Given that generic 15 mg meloxicam remains affordable, typically retailing between $25 and $45 for a 30-day supply in 2026, it serves as a pragmatic, first-line choice for long-term management.
Conversely, when managing acute, transient flare-ups, the rapid onset of ibuprofen—which usually provides relief within 30 to 60 minutes—remains superior. However, because its effects dissipate in just 4 to 6 hours, it is often suboptimal for chronic conditions. Clinicians must emphasize that combining these two agents is strictly contraindicated, as concurrent use significantly elevates the risk of gastrointestinal ulcers and nephrotoxicity. Furthermore, while the evolution toward COX-2 selective agents like meloxicam was designed to mitigate such GI risks, caution remains necessary, particularly regarding cardiovascular safety in aging populations and pregnancy, where NSAIDs should be avoided after 20 weeks of gestation. By matching the medication’s pharmacokinetics to your specific needs, you and your physician can balance efficacy with safety, ensuring a sustainable approach to pain management. Written by Frankie Sze.



