Is Meloxicam Addictive? Understanding Non-Narcotic Pain Relief
By Frankie Sze | 5/2/2026
The Opioid Shadow: Why Patients Fear Prescription Painkillers
In the wake of an ongoing national opioid crisis, a pervasive cultural anxiety has taken root, causing many patients to view all prescription-strength pain management with profound skepticism. This hesitation is understandable, yet it often creates a barrier to effective care. Modern clinical guidelines, updated in 2026, now mandate that clinicians prioritize shared decision-making to explain the fundamental safety and pharmacological profiles of non-opioid alternatives, such as meloxicam. Unlike narcotics, meloxicam is a non-narcotic NSAID that does not trigger dopamine release in the mesolimbic reward pathway, meaning it is not considered addictive. Patients often grapple with the complexities of these choices; as noted by clinical experts, “Patients frequently wonder whether meloxicam or ibuprofen works better for arthritis pain, how quickly each provides relief, and how often they must be taken.”
Understanding the distinction between classes of medication is vital for long-term health. While opioids carry the weight of dependency, the primary risks associated with misusing meloxicam involve physiological outcomes, such as gastrointestinal bleeding or kidney damage, rather than psychological cravings. Typically dosed once daily at 7.5 mg to 15 mg for sustained anti-inflammatory control, meloxicam serves as a cornerstone of the modern movement toward multimodal pain plans that reserve opioids only as a final resort. It is important to note that while the medication is non-addictive, stopping it may lead to rebound inflammation within 24 hours to one week, necessitating steady adherence. To better understand how this therapy works in practice, readers can consult our Meloxicam 101: Your Daily Guide to Steady Joint Relief. As 2026 guidelines solidify NSAIDs as the first-line pharmacologic choice for chronic pain, patients can transition away from the ‘opioid shadow’ toward safer, sustainable relief.

NSAIDs vs. Narcotics: A Fundamental Difference in Chemistry
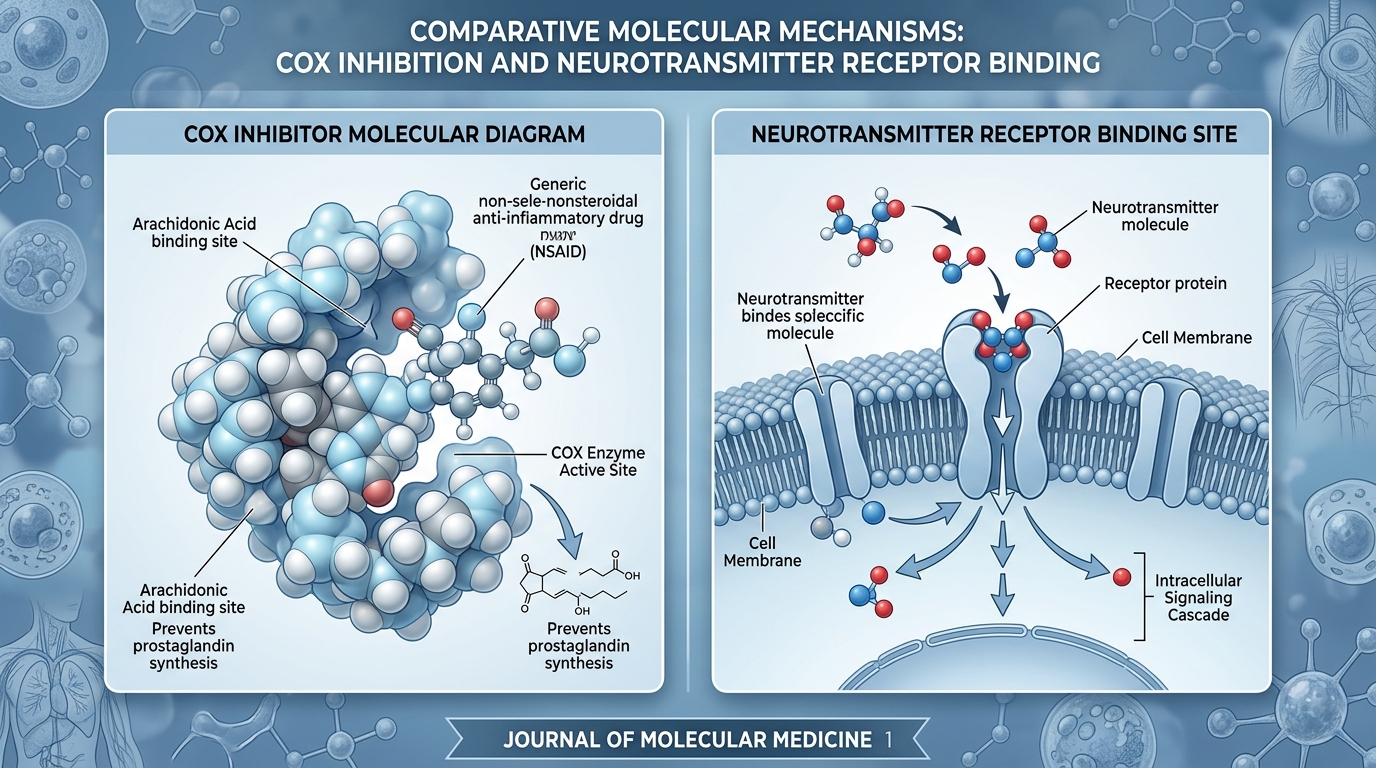
To understand why the medical community has shifted away from opioid-centric pain management, we must look at the divergent chemical pathways of these medications. Narcotics, or opioids, exert their analgesic effects by binding to mu-receptors in the central nervous system, which triggers a significant dopamine release in the mesolimbic reward pathway—the biological trigger for addiction. In contrast, non-steroidal anti-inflammatory drugs (NSAIDs) like meloxicam function by inhibiting the cyclooxygenase (COX) enzymes, thereby reducing the production of prostaglandins that mediate inflammation and pain. As noted by the Ikon Recovery Centers, “Neither meloxicam nor ibuprofen is considered addictive, though both carry risks of serious side effects when misused or taken in excessive amounts.”
The cultural shadow cast by the opioid crisis has fostered a persistent fear of all prescription-strength pain relief, yet 2026 clinical guidelines explicitly recommend NSAIDs as the first-line pharmacologic choice for chronic pain precisely to prevent dependence. Unlike opioids, meloxicam is not a narcotic; its misuse poses distinct physiological threats, specifically gastrointestinal bleeding and kidney damage, rather than the psychological cravings associated with controlled substances. While stopping meloxicam—typically dosed once daily at 7.5 mg to 15 mg for sustained anti-inflammatory control—can lead to rebound inflammation within 24 hours to one week, this is a physiological withdrawal from therapy rather than a behavioral addiction.
Current clinical protocols urge clinicians to utilize shared decision-making to clarify these chemical distinctions for patients. As we look toward a future defined by multimodal pain plans, the medical hierarchy is clear: opioids are reserved as a last resort, prioritizing the safety of non-addictive, mechanism-specific alternatives like meloxicam.
The Science of No ‘High’: Why Meloxicam Skips the Reward System
In the wake of an opioid crisis that fostered a deep, systemic fear of prescription-strength pain management, patients and clinicians alike are re-evaluating the profile of non-narcotic alternatives. A primary point of confusion remains the distinction between pain relief and euphoria. As Frankie Sze, I often emphasize that while opioids operate by hijacking the brain’s mesolimbic reward pathway—triggering dopamine release to create a ‘high’—meloxicam functions entirely outside this framework. As noted by able2changerecovery.com, “Unlike opioids, meloxicam does not interact with the central nervous system in the same way, eliminating the potential for a euphoric high.”
Because meloxicam does not stimulate dopamine, it does not induce psychological dependence or the addictive cravings characteristic of narcotic analgesics. Instead, its mechanism is purely peripheral, targeting inflammation directly. Given this safety profile, 2026 clinical guidelines now recommend NSAIDs like meloxicam as the first-line pharmacologic choice for chronic pain, positioning them as the foundation of future multimodal pain management plans where opioids are reserved only as a final, last-resort option. Clinicians are encouraged to engage in shared decision-making to explain these safety nuances to patients, clarifying that while misuse of meloxicam does not lead to a ‘high,’ it does carry serious risks, such as gastrointestinal bleeding and kidney damage, rather than addiction.
Patients should be aware that while meloxicam lacks the withdrawal symptoms associated with chemical dependency, its discontinuation can result in a resurgence of physical symptoms. Stopping the medication, which is typically dosed once daily at 7.5 mg to 15 mg for sustained control, may cause rebound inflammation within 24 hours to one week. By clearly separating the physiological reality of inflammation management from the psychological risks of narcotic abuse, we can empower patients to utilize meloxicam safely and effectively within their long-term wellness strategy.
Dependence vs. Necessity: Taking Meloxicam for Chronic Conditions
In the wake of the opioid crisis, a profound cultural apprehension has emerged regarding the use of any prescription-strength pain medication. However, it is essential to distinguish between the physiological requirement of a chronic disease treatment and the psychological compulsion characteristic of substance use disorder. Meloxicam, a non-narcotic NSAID, is fundamentally non-addictive; unlike opioids, it does not trigger the dopamine release associated with the mesolimbic reward pathway. As The Freedom Center notes, “Meloxicam offers once-daily dosing with longer-lasting effects, making it preferred for chronic inflammatory conditions like arthritis.”
By 2026, medical guidelines have shifted to prioritize shared decision-making, encouraging clinicians to clarify that daily adherence to a 7.5 mg to 15 mg meloxicam regimen is a standard medical routine for managing mobility and inflammation. While the medication does not induce addiction, stopping it abruptly can lead to a return of symptoms, as patients may experience rebound inflammation within 24 hours to one week. It is crucial to understand that misuse of meloxicam does not result in the cravings seen in chemical dependency; rather, it significantly elevates risks for gastrointestinal bleeding and kidney damage. Moving forward, clinical frameworks are increasingly adopting multimodal pain plans that reserve opioids as a last resort, positioning NSAIDs as the first-line pharmacologic choice to ensure both patient safety and effective long-term symptom management.
Misuse is Not Addiction: Understanding the Real Risks of Overuse
In the wake of an opioid crisis that fostered a deep, systemic anxiety surrounding all prescription-strength analgesics, patients often conflate the concept of dependence with the necessity of daily medication. It is critical to distinguish that meloxicam—a non-narcotic NSAID—is not addictive. Unlike opioids, meloxicam does not trigger dopamine release in the mesolimbic reward pathway, meaning it carries no inherent risk for psychological cravings or chemical dependency. As of 2026, clinical guidelines firmly recommend NSAIDs as first-line pharmacologic choices for chronic pain management specifically to avoid the pitfalls of opioid dependence.
However, the absence of addiction potential should not be mistaken for a mandate for unmonitored use. Meloxicam is typically dosed once daily at 7.5 mg to 15 mg to provide sustained anti-inflammatory control, and deviating from this prescribed regimen presents significant physiological hazards. According to clinical guidance, “Doing so can increase the risk of serious side effects, complications, and overdose.” Misuse of meloxicam elevates the risk of life-threatening gastrointestinal bleeding and acute kidney damage, outcomes far more medically urgent than the addiction concerns associated with controlled substances.
Furthermore, patients should be aware of the physical “rebound” phenomenon. Abruptly ceasing the medication can lead to a resurgence of inflammation within 24 hours to one week as the body’s baseline inflammatory response returns. Moving forward, the standard of care relies on multimodal pain plans—where clinicians and patients use shared decision-making to clarify that non-opioid alternatives like meloxicam are safer tools that reserve opioids strictly as a last resort. Understanding that the risk of meloxicam lies in physical harm from over-dosage, rather than a cycle of addiction, is essential for patients to safely manage their chronic conditions.
Stopping Treatment: Rebound Pain vs. Withdrawal Symptoms
In the wake of the opioid crisis, a lingering cultural apprehension toward all prescription-strength pain management often clouds the clinical picture. However, it is essential to distinguish between the physiological return of underlying symptoms and the psychological cravings associated with addictive substances. Meloxicam is a non-narcotic NSAID; unlike opioids, it does not trigger dopamine release in the mesolimbic reward pathway and is not considered addictive. As noted by experts at BetterAddictionCare, “When someone stops meloxicam suddenly—especially after long-term use—the body may react. It’s not withdrawal in the addictive sense, because meloxicam doesn’t change brain reward pathways or create cravings.”
Patients who discontinue their daily 7.5 mg to 15 mg dosage often confuse this biological reality with drug withdrawal. In truth, stopping meloxicam may trigger a recurrence of rebound inflammation within 24 hours to one week as the anti-inflammatory effects subside. This return of pain is a signal that your original condition requires continued management, not a symptom of dependence. Misuse of the medication carries risks to gastrointestinal and kidney health rather than the psychological cravings seen in dependency cycles. To ensure consistent efficacy, it is vital to follow established protocols, as discussed in Meloxicam 101: Your Daily Guide to Steady Joint Relief.
As of 2026, clinical guidelines firmly recommend NSAIDs as first-line pharmacologic choices for chronic pain to avoid the hazards of opioid dependence. By utilizing shared decision-making, clinicians and patients are moving toward future-facing, multimodal pain plans that reserve opioids only as a final resort. Understanding that your body is responding to a lack of inflammation suppression—rather than withdrawal—is the first step in effective, long-term pain management.



