Can I Take Meloxicam with Ibuprofen? Safety and Risks
By Frankie Sze | 5/2/2026
The NSAID Family Tree: Why Meloxicam and Ibuprofen are Relatives
When managing chronic inflammation, it is easy to view medication as distinct tools in a toolbox, but in reality, some choices overlap in ways that can threaten patient safety. As noted in clinical guidelines, “Both meloxicam and ibuprofen belong to the class of medicines known as nonsteroidal anti-inflammatory drugs (NSAIDs).” While meloxicam is typically dosed once daily at 7.5 mg to 15 mg for chronic conditions like arthritis, ibuprofen is generally reserved for acute flares, requiring dosing every 4 to 6 hours. For those currently navigating their treatment plan, our Meloxicam 101: Your Daily Guide to Steady Joint Relief offers a deeper look at why consistency is key for this medication.
The biological rationale for their relationship stems from the discovery of COX-1 and COX-2 enzymes. Scientists developed meloxicam to be more COX-2 selective than ibuprofen, aiming to mitigate the stomach irritation long associated with the class; however, both still carry significant gastrointestinal risks. Combining these agents is strictly contraindicated, as doing so multiplies the risk of severe gastrointestinal bleeding and acute kidney failure. If you are transitioning between therapies, strict safety windows apply: a 6-hour wait is required after taking ibuprofen before starting meloxicam, while a full 24-hour buffer is mandatory after a meloxicam dose before introducing ibuprofen. For breakthrough pain, clinicians often suggest acetaminophen (Tylenol), which does not interact with the NSAID pathway. As clinicians increasingly shift toward long-term strategies like physical therapy to reduce medication reliance, it is essential to remember that even familiar over-the-counter options are powerful agents that should never be stacked.

The Double-Dosing Trap: Why One Plus One Doesn’t Equal Double Relief
Patients frequently assume that layering medications will accelerate recovery, but when managing chronic arthritis with meloxicam and acute flares with ibuprofen, this strategy is medically counterproductive. Meloxicam is typically dosed once daily at 7.5 mg to 15 mg, whereas ibuprofen is commonly taken every 4 to 6 hours in 200 mg to 400 mg increments. While the discovery of COX-1 and COX-2 enzymes once spurred the development of selective inhibitors like meloxicam to mitigate gastric irritation, it is a clinical misconception that combining these two agents provides superior pain relief. In reality, combining two NSAIDs simply multiplies the risk of gastrointestinal bleeding and kidney failure. According to Ikon Recovery Centers, “Doing so can increase the risk of serious side effects, complications, and overdose.”
Although meloxicam is more COX-2 selective than ibuprofen, it still carries significant GI risks that are compounded by the addition of another NSAID. Strict temporal buffers are essential for safety: a 6-hour wait is required after taking ibuprofen before starting meloxicam, while a 24-hour wait is mandatory after a meloxicam dose before introducing ibuprofen. For patients requiring relief from breakthrough pain, acetaminophen (Tylenol) serves as a safer, non-interacting alternative, as it does not share the same renal or gastric pathways as NSAIDs. As clinicians increasingly pivot toward non-drug therapies like physical therapy to reduce long-term reliance on these medications, it is vital to recognize that more is rarely better—it is only more dangerous.

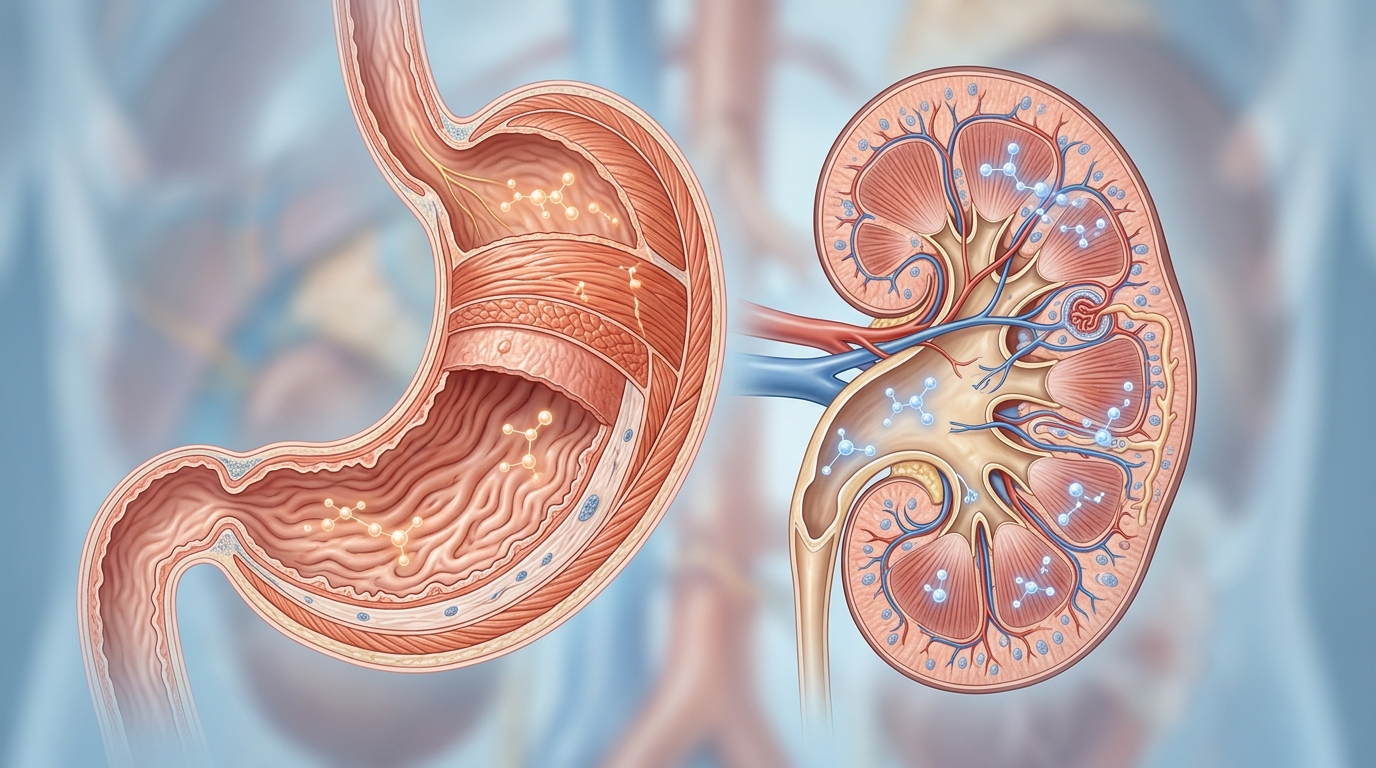
Internal Impact: How the Stomach and Kidneys React to Overload
While the discovery of COX-1 and COX-2 enzymes once promised a new era of safer pain management—leading to the development of selective agents like meloxicam—the clinical reality of NSAID therapy remains precarious. Meloxicam, typically dosed once daily at 7.5 mg to 15 mg, offers a degree of COX-2 selectivity compared to the more frequent 200 mg to 400 mg dosing regimen of ibuprofen; however, neither is exempt from systemic risk. When patients attempt to layer these medications, the physiological strain on the gastric mucosa and renal system becomes significant.
The kidneys rely on prostaglandins to maintain adequate renal blood flow, particularly in sensitive populations. Excessive COX inhibition restricts this blood flow, potentially leading to acute injury. As noted by clinical guidance, “Because both medications are NSAIDs, taking them together increases the risk of side effects, such as stomach ulcers, gastrointestinal bleeding, or kidney damage.” The combined toxicity is not merely additive; it is multiplicative, overwhelming the stomach’s protective lining and the kidneys’ filtration homeostasis.
For those managing chronic arthritis with meloxicam alongside acute flare-ups, strict adherence to temporal spacing is essential to mitigate harm. A minimum six-hour buffer is required after taking ibuprofen before initiating meloxicam, and a 24-hour wash-out period is mandated when switching from meloxicam to ibuprofen. For patients requiring relief from breakthrough pain, acetaminophen remains the standard, as it does not interfere with the COX-inhibition pathways of these drugs. Moving forward, clinicians are increasingly recommending non-drug therapies like physical therapy to reduce the long-term reliance on NSAIDs and preserve both gastric and renal integrity.
I Accidentally Took Both: Immediate Steps and Red Flags
If you have inadvertently combined meloxicam—typically prescribed as a once-daily dose of 7.5 mg to 15 mg—with ibuprofen, which is generally taken in 200 mg to 400 mg increments every 4 to 6 hours, you have significantly elevated your risk profile. While the medical community historically shifted toward selective NSAIDs like meloxicam to minimize COX-1 related gastric irritation, doubling up on these agents compounds the threat of gastrointestinal hemorrhaging and acute kidney injury. To maintain safety, clinical guidelines mandate a 6-hour waiting period after ibuprofen consumption before starting meloxicam, and a full 24-hour buffer after a meloxicam dose before introducing ibuprofen.
Should you realize you have taken both, monitor your body closely. According to Brooks Healing Center, concerning clinical signs “can include: Nausea and vomiting, Severe stomach pain, Drowsiness or lethargy, Ringing in the ears (tinnitus), Dizziness and blurred vision, Difficulty breathing.” If these symptoms manifest, seek emergency medical attention immediately. While chronic conditions like arthritis often require consistent management, remember that acetaminophen (Tylenol) does not share the same mechanism of action as NSAIDs and serves as a safer alternative for breakthrough pain without these specific risks. As we look toward future care standards, clinicians are increasingly prioritizing non-pharmacological modalities, such as physical therapy, to decrease the long-term reliance on multiple anti-inflammatory agents.
Safe Alternatives: Managing Breakthrough Pain the Right Way
When managing chronic arthritis, meloxicam is typically dosed once daily at 7.5 mg to 15 mg to provide steady, long-acting relief. However, patients may still experience breakthrough pain that standard daily dosing does not fully address. It is a common misconception that adding an over-the-counter NSAID like ibuprofen—often taken in 200 mg to 400 mg doses every 4 to 6 hours—will provide a safe boost. In reality, combining two NSAIDs significantly multiplies the risk of gastrointestinal bleeding and kidney failure. While meloxicam is more COX-2 selective than ibuprofen, it still carries significant GI risks that preclude simultaneous use with other non-steroidal anti-inflammatories.
To ensure safety, patients must adhere to strict washout periods if switching between these medications: a 6-hour wait is required after taking ibuprofen before starting meloxicam, and a 24-hour wait is necessary after taking meloxicam before switching to ibuprofen. Because these risks are so pronounced, clinicians consistently look for safer, non-NSAID alternatives for acute flare-ups. As noted by medical experts, “Because meloxicam is long-acting, acetaminophen can help control breakthrough pain without raising NSAID risks.” Clinical data indicates that acetaminophen (Tylenol) does not interact with the meloxicam pathway, making it the preferred, clinically recommended option for managing breakthrough pain without compromising systemic safety.
The Waiting Game: How to Safely Switch from Ibuprofen to Meloxicam
Transitioning between non-steroidal anti-inflammatory drugs (NSAIDs) requires strict adherence to timing to prevent dangerous interactions. Because both ibuprofen—typically dosed at 200 mg to 400 mg every 4 to 6 hours—and meloxicam, a once-daily medication ranging from 7.5 mg to 15 mg, act on similar bodily systems, combining them exponentially increases your risk of gastrointestinal bleeding and acute kidney failure. While meloxicam is more COX-2 selective than the older ibuprofen, it still carries significant internal risks, making the transition window critical.
If you are moving from an acute regimen of ibuprofen to the steady, once-daily management described in Meloxicam 101: Your Daily Guide to Steady Joint Relief, you must observe a mandatory washout period. According to clinical guidance found at Drugs.com, “For most people, that’s about 6 hours after the last dose of ibuprofen” before you can safely initiate your first dose of meloxicam. Conversely, if you are currently taking meloxicam and find it insufficient for a specific flare, you must wait a full 24 hours after your last meloxicam dose before returning to ibuprofen to avoid toxic accumulation in your system.
For those managing breakthrough pain during these waiting periods, clinicians often suggest acetaminophen (Tylenol), which does not interact with the COX-inhibition pathways of NSAIDs and can be used as a safer stopgap. As we look toward the future of pain management, clinicians are increasingly recommending non-drug therapies like physical therapy to reduce the long-term reliance on these powerful medications and mitigate the risk of systemic inflammation.



