Sleeping Through Arthritis Pain: Meloxicam for Nighttime Relief
By Frankie Sze | 5/2/2026
The Nighttime Arthritis Trap: Why Joint Pain Peaks at Rest
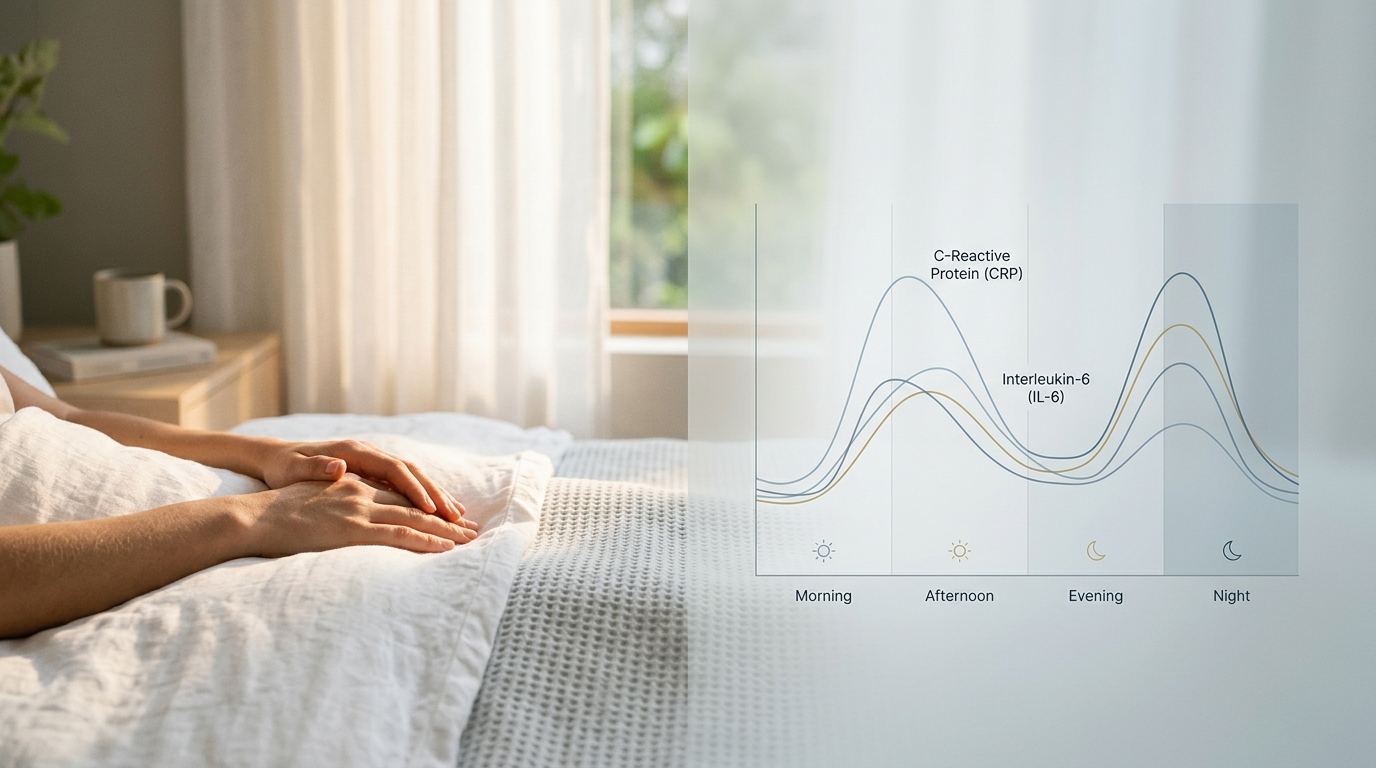
For millions living with rheumatoid arthritis, the transition from evening to early morning is not a period of restorative rest, but a window of heightened vulnerability. Clinical data confirms that 65.3% of rheumatoid arthritis patients report significant sleep disturbances, a cycle that becomes self-perpetuating, as a single night of fragmented sleep can lower pain thresholds by approximately 15%. This phenomenon is rooted in the body’s internal clock; as established by research, “Pro-inflammatory cytokines such as interleukin-6, tumor-necrosis factor-alpha and interleukin-1beta follow a clear 24-hour pattern in rheumatoid arthritis, reaching their highest concentrations during the late-night to early-morning hours (approximately 02:00–06:00) when plasma cortisol, the main endogenous anti-inflammatory hormone, is at its nadir,” as noted in this clinical study on cytokine periodicity.
Historically, traditional arthritis management relied on short-acting NSAIDs that necessitated frequent dosing. Because common options like ibuprofen typically wear off after four to six hours, patients were left unprotected during the critical 02:00 to 06:00 surge, often waking to debilitating breakthrough pain. In contrast, current clinical strategies emphasize the role of circadian rhythms in inflammation, favoring long-acting medications designed for 24-hour coverage. For those seeking consistency, Meloxicam 101: Your Daily Guide to Steady Joint Relief explores how pharmacological timing can mitigate these symptoms. Meloxicam is typically dosed once daily at 7.5 mg to 15 mg, leveraging its long half-life to provide sustained suppression of inflammatory markers throughout the night. To optimize this approach, taking the medication with food can decrease associated gastrointestinal side effects by up to 40%. Looking ahead, the field is shifting toward personalized chronotherapy protocols, which aim to align medication delivery precisely with an individual’s unique cytokine profile to ensure that relief is not merely reactive, but perfectly timed.

Steady-State Relief: How Meloxicam’s Half-Life Prevents Breakthrough Pain
Historically, arthritis management relied on short-acting non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen, which typically provide therapeutic effects for only 4 to 6 hours. This necessitated frequent dosing, frequently resulting in ‘wearing off’ periods overnight that left patients vulnerable to breakthrough pain. The clinical landscape has since shifted toward recognizing the critical role of circadian rhythms in inflammatory pathology; notably, pro-inflammatory cytokines reach their peak concentrations between 02:00 and 06:00, a time when traditional medications have long been metabolized. This is particularly concerning given that 65.3% of rheumatoid arthritis patients are classified as poor sleepers, and even a single night of fragmented sleep can lower pain thresholds by approximately 15%.
To combat these nocturnal troughs, clinicians now favor agents like meloxicam, which is typically dosed once daily at 7.5 mg to 15 mg. Due to its pharmacokinetic profile, its longer half-life means the medication stays active throughout the day, providing consistent pain relief. This sustained effect makes meloxicam particularly practical for managing ongoing arthritis pain. By maintaining a steady-state plasma concentration, meloxicam mitigates the risk of sudden pain recurrence. To further optimize treatment outcomes and enhance tolerability, patients are advised that taking meloxicam with food can decrease gastrointestinal side effects by up to 40%. Looking ahead, the medical community is moving toward personalized chronotherapy protocols, aiming to align medication timing precisely with individual cytokine profiles to ensure comprehensive, 24-hour symptom control.

The Sleep-Recovery Connection: How Rest Impacts Joint Health
For individuals managing chronic joint inflammation, the relationship between rest and pain regulation is far from passive. Clinical data reveals a concerning prevalence of sleep disturbances within this population, with 65.3% of rheumatoid arthritis patients classified as poor sleepers. This is particularly problematic because of the body’s circadian biology; pro-inflammatory cytokines reach peak concentrations between 02:00 and 06:00, often coinciding with the early morning stiffness that defines the patient experience. Historically, traditional arthritis management relied on short-acting NSAIDs like ibuprofen, which generally wear off after four to six hours, often leaving patients vulnerable to breakthrough pain during these critical overnight windows.
The physiological cost of disrupted rest is substantial. In one study of healthy young adults, a single night of poor sleep reduced their pain threshold by 15%, a statistic that underscores the direct link between sleep deprivation and exacerbated pain sensitivity. Current clinical strategies have shifted to account for these rhythms, favoring long-acting NSAIDs such as meloxicam to provide consistent, 24-hour symptom control. Typically dosed once daily at 7.5 mg to 15 mg, meloxicam’s long half-life offers a more stable therapeutic profile than legacy medications. Furthermore, to improve patient adherence and mitigate systemic irritation, clinical guidelines suggest that taking meloxicam with food can decrease gastrointestinal side effects by up to 40%. Looking ahead, the field is moving toward personalized chronotherapy, where medication timing will be precisely calibrated to align with an individual’s unique cytokine profile.
Optimizing Your Routine: Timing Your Dose for a Better Night’s Sleep
For patients navigating the persistent discomfort of rheumatoid arthritis, the management of nighttime inflammation is often the final hurdle in achieving restorative rest. Historically, arthritis treatment relied on short-acting NSAIDs like ibuprofen, which typically provide relief for only four to six hours. This frequent dosing requirement often resulted in gaps of protection, leaving patients vulnerable to ‘wearing off’ periods that manifest as breakthrough pain during the small hours of the morning. This is particularly problematic given that pro-inflammatory cytokines reach their peak concentrations between 02:00 and 06:00, a window that coincides with the most common timing for sleep disruption. Because a single night of fragmented sleep can lower pain thresholds by approximately 15%, the biological impact of these nighttime gaps is profound, especially when considering that 65.3% of rheumatoid arthritis patients are classified as poor sleepers.
Current research emphasizes the critical role of circadian rhythms in inflammation, leading to a shift toward long-acting NSAIDs like meloxicam, which are typically prescribed at 7.5 mg to 15 mg once daily. By leveraging the medication’s extended half-life, patients can achieve more consistent 24-hour symptom control. As noted in guidance from Bezzy RA, “If you have more RA-related pain at night or experience severe morning stiffness, taking meloxicam later in the evening may help manage these symptoms.” When shifting your dosing to the evening, remember that taking meloxicam with a light snack or food can decrease gastrointestinal side effects by up to 40%, ensuring your comfort without compromising efficacy.
Looking toward the future, clinical focus is shifting to personalized chronotherapy, where dosing schedules are calibrated to align medication peaks with an individual’s specific cytokine profile. By proactively managing the inflammatory rhythm rather than simply reacting to pain, patients can better secure the quality sleep essential for long-term health. As always, consult your rheumatologist before adjusting your medication timing to ensure the protocol is safe for your specific health needs.
Breaking the Cycle: From Better Sleep to Better Morning Mobility
Breaking the cycle of chronic pain requires addressing the physiological reality of the overnight period. With pro-inflammatory cytokines reaching peak concentrations between 02:00 and 06:00, the body is most vulnerable during the early morning hours. This reality is particularly stark for the 65.3% of rheumatoid arthritis patients who are classified as poor sleepers. When sleep is fragmented, research indicates that pain thresholds can drop by approximately 15%, turning a manageable condition into an exhausting cycle of hypersensitivity. Unlike traditional management with ibuprofen, which typically wears off after 4 to 6 hours and often triggers breakthrough pain at night, modern care focuses on circadian-synchronized treatment.
As noted by Doctronic experts, “Meloxicam excels for chronic inflammatory conditions like rheumatoid arthritis requiring consistent relief throughout the day and night.” By providing 24-hour symptom control, long-acting NSAIDs like meloxicam help patients bypass the dawn-surge of inflammation that so often leads to severe morning stiffness. Patients should remember that meloxicam is typically dosed once daily at 7.5 mg to 15 mg to maintain this stable concentration, and taking it with food can decrease gastrointestinal side effects by up to 40%. For more on managing your routine, consult our guide at Meloxicam 101: Your Daily Guide to Steady Joint Relief.
Looking ahead, the shift toward personalized chronotherapy will further align medication timing with individual cytokine profiles, ensuring that the inflammatory response is blunted before it even begins. By stabilizing your sleep, you create a positive feedback loop: better sleep reduces inflammation, which in turn preserves physical function, allowing for greater mobility the following morning. Through proactive, consistent pharmacological support, patients can move beyond reactive dosing and achieve a more stable, higher quality of life.


